Key takeaways:
~ Adenosine is key to slow-wave sleep, and the rate at which you break down adenosine impacts your sleep quality.
~ BDNF, a brain-derived neurotrophic factor, is also important here.
~ A variant in the ADA gene (adenosine deaminase) changes the rate at which adenosine is metabolized during sleep. This affects how much sleep you need each night in order to clear out excess adenosine.
Why is slow-wave sleep important?
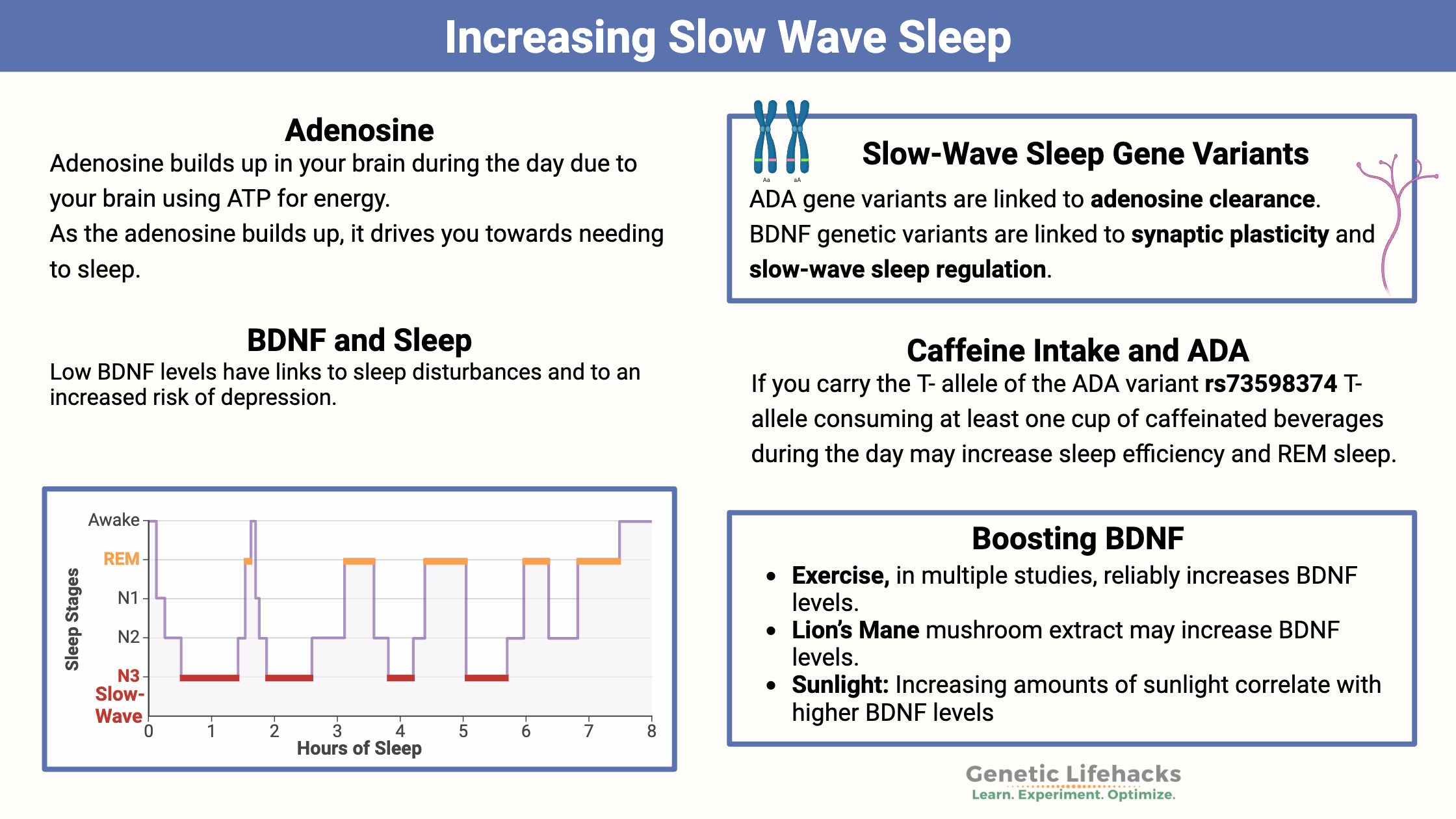
When you sleep, your brain goes through different electrical wave patterns. Part of the time, you will have REM sleep, which is characterized by rapid eye movement and higher-frequency brain waves. Non-REM sleep cycles include brain activity at lower frequencies.
Non-REM slow-wave sleep is important for memory consolidation. When you are awake, memories are stored temporarily in the hippocampus, but during non-REM slow-wave sleep, those memories are transferred to the neocortex for long-term storage.[ref]
Non-REM sleep has 3 stages:
- Stage 1 is the beginning of sleep – just when you are drifting off.
- Stage 2 is a lighter stage of sleep- easy to be woken up
- Stage 3 is the deep, slow-wave sleep
Adenosine and Slow Wave Sleep:
Sleep is thought to be initiated by two different processes: your circadian rhythm (24-hour, built-in clock) and homeostatic sleep drive.
The homeostatic sleep drive is what makes you feel sleepy, and adenosine is a key player here.
Adenosine builds up in your brain during the day due to your brain using ATP (adenosine triphosphate) for energy. The ATP molecule gives up a phosphate as a way to produce energy from the chemical bond. This then creates ADT (adenosine diphosphate) which can then give up another phosphate to become AMP (adenosine monophosphate). The final step leaves the cell with just adenosine. As the adenosine builds up, it drives you towards needing to sleep.
The adenosine receptor, ADORA2A, is what adenosine attaches to and plays a crucial role in the homeostatic sleep drive. If you block the adenosine receptor, you will feel more alert. This is how caffeine works – it attaches to ADORA2A, blocking adenosine from the receptor.
Adenosine levels drop as you sleep:
One way that the body can control adenosine levels is to convert them to inosine using the enzyme adenosine deaminase (ADA gene). This enzyme helps to metabolize adenosine while you sleep, resulting in lower adenosine levels when you wake.[ref] As the adenosine levels drop over the course of the night, the pressure to sleep also decreases.[ref] Genetic variants that affect the function of the ADA gene are linked to feeling groggy in the morning when not getting sufficient sleep.
While researchers have known for a while that adenosine is important in feeling sleepy, recent animal studies have clearly shown that activation of the adenosine receptor, ADORA2A, by the adenosine molecule, induces slow-wave sleep.[ref]
BDNF and Sleep:
BDNF (brain-derived neurotrophic factor) acts within the brain to potentiate or increase, synaptic connections between neurons. One of the roles of BDNF is to help with neuroplasticity and memory formation.
It turns out that BDNF may also be important in slow-wave sleep. Low BDNF levels have links to sleep disturbances and to an increased risk of depression.[ref]
Genetic variants that affect slow wave sleep:
A common BDNF genetic variant, known as Val 66Met (below), is linked to alterations in slow-wave sleep. A recent study showed that Val/Val carriers average 20 minutes deeper slow-wave sleep than people with a Met allele. Val/Val carriers also have higher average BDNF levels.[ref]
There is a genetic variant in the adenosine deaminase (ADA) gene that decreases the clearance rate of adenosine. People who carry the variant get more slow-wave, deep sleep at night on average. The flip side is that a short night’s sleep may leave them feeling groggy the next day.
Slow Wave Sleep Genotype Report:
Access this content:
An active subscription is required to access this content.
Lifehacks:
If you have a way to track your slow-wave sleep, you may want to experiment with some of the options below to see if you can affect the amount of time that you spend in a deep sleep.
Caffeine Intake and ADA:
Access this content:
An active subscription is required to access this content.
Related Articles and Topics:
Problems sleeping? Your genes can point to individualized solutions
References: