Key takeaways:
- The blood-brain barrier (BBB) prevents circulating toxins and pathogens from reaching the brain.
- Tight junctions between the epithelial cells and specific transporters keep the brain isolated and protected.
- Certain genetic variants increase your risk of BBB dysfunction.
- Blood-brain barrier dysfunction can be part of the cause of Alzheimer’s, depression, and neurological disorders.
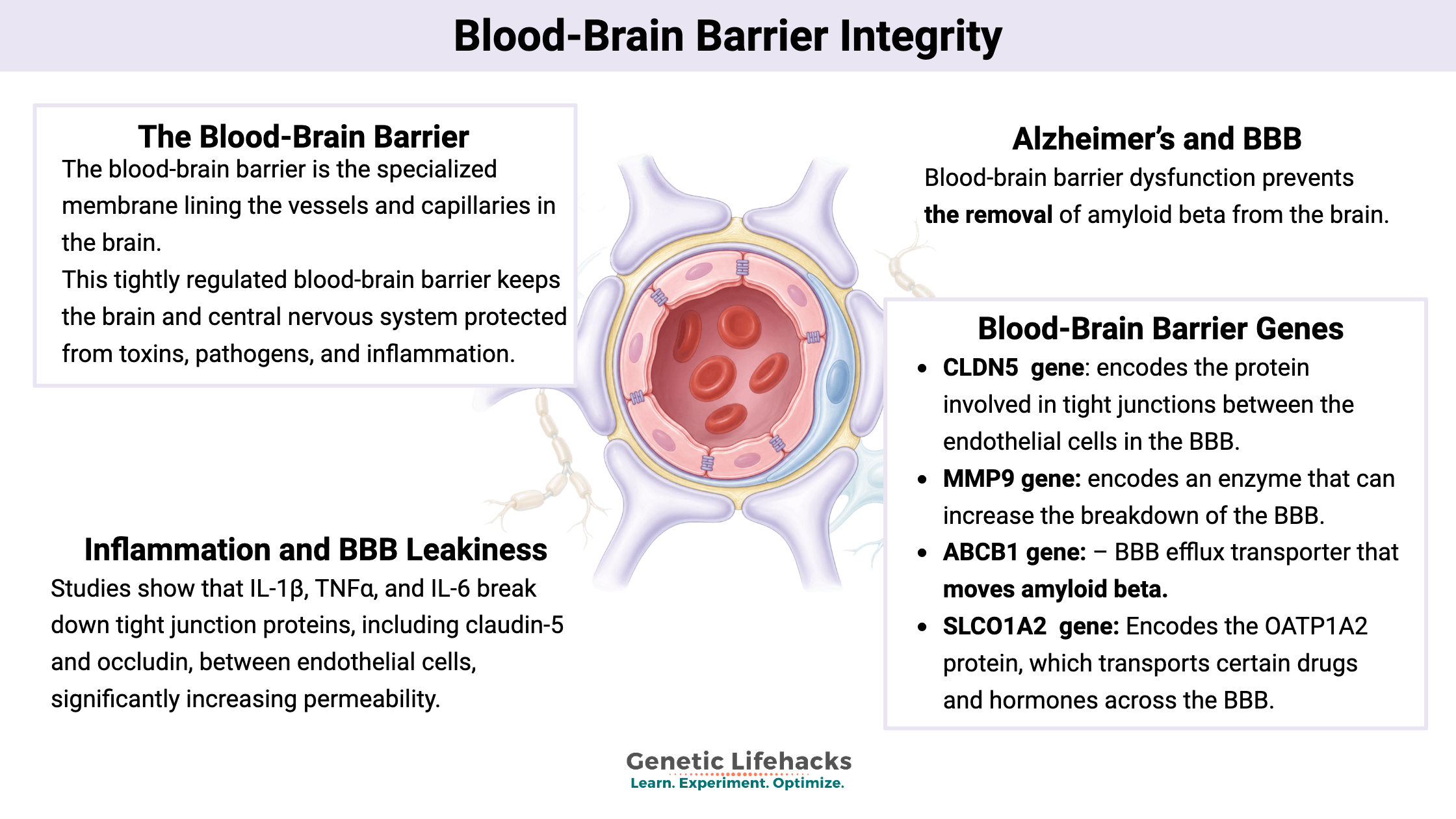
What is the blood-brain barrier?
The blood-brain barrier is the term for the specialized membrane lining the vessels and capillaries in the brain. The blood vessels that move blood to the brain are unique in how they allow molecules to move through them.
This specialized semipermeable membrane tightly regulates what can pass through to the brain – and move out of the brain – with tight junctions between the cells lining the blood vessels. There are specific transporters in this barrier that regulate what can pass through it, to and from the brain.[ref][ref]
This tightly regulated blood-brain barrier keeps the brain and central nervous system protected from toxins, pathogens, and inflammation.
Capillaries: Capillaries are the small blood vessels that branch out throughout the brain, and they make up the majority of the blood-brain barrier. In the capillaries, the endothelial cells that line these tiny vessels are tightly wedged together. They allow oxygen and glucose into the brain while transporting out metabolic waste. These tight junctions in the BBB also prevent 98% of drugs from passing through to the brain.[ref]
Endothelial cells: The cells lining the blood vessels, endothelial cells, are joined together with tight junctions that prevent molecules from slipping through. In addition, the endothelium also contains transporters for actively transporting the nutrients and amino acids needed by the brain.
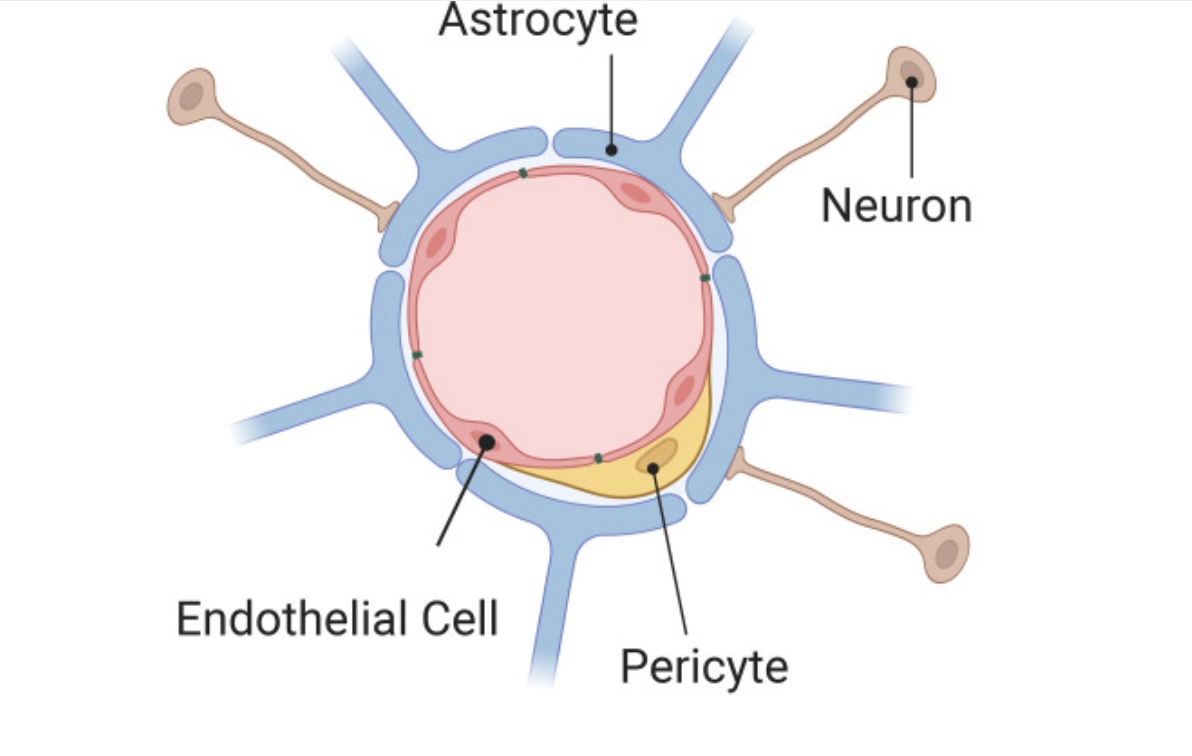
Surrounded by specialized cells: These tiny capillaries that supply the brain are surrounded by astrocytes, pericytes, and microglia – specialized types of brain cells that support and protect the neurons that make up the brain.[ref]
Together, this is called a neurovascular unit.
A little history –
The blood-brain barrier was discovered in the 1880s by the German microbiologist Paul Ehrlich. He was injecting animals with blue dye to determine the organ distribution, and he found that the brain and other parts of the central nervous system remained unaffected. While this was considered one of the first experiments referring to the physiology of the barrier, the term wasn’t used until 1921.[ref]
Structure of the BBB:
The endothelial cells lining the capillaries are tightly bound together with tight junctions formed by proteins called claudins and occludins. The endothelial cells that line the brain vessels have a flatter shape and tighter connections compared to the endothelial cells in blood vessels throughout the rest of the body. They also lack the small pores that are found in other parts of the endothelium.
The neurovascular unit includes endothelial cells, astrocytes, pericytes, and neurons, all working together to regulate what enters the brain and how waste products are removed from the central nervous system.[ref]
What can pass through the BBB?
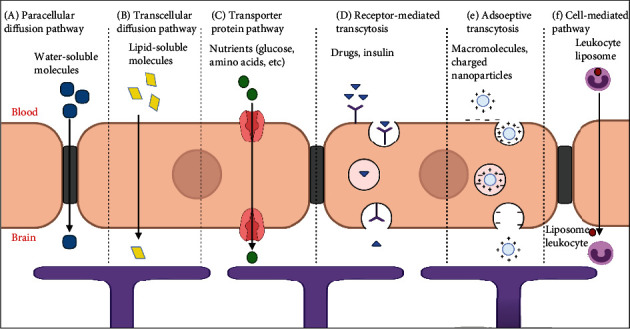
The brain needs energy, oxygen, and nutrients, and these can pass through the BBB in different ways.[ref]
- Small, lipid-soluble molecules such as oxygen and carbon dioxide can cross the BBB through passive transport.
- Glucose and certain amino acids can pass through the BBB with a carrier-mediated transport process.
- Hormones and insulin are moved through as needed.
- Large molecules can be moved through the BBB through selective cell surface receptors that bind to the specific molecules to move them into the cell through endocytosis.
Transporters found in the BBB:
ABC Transport proteins are a family of transporters that use ATP to pump molecules across membranes, including the BBB. ABCB1, ABCC1, and ABCG2 are transporters found in the BBB that are important for delivering drugs to the brain. These transporters can also move metabolic waste out of the brain.
Organic anion transporting polypeptides (OATPs) move specific organic substrates across the BBB. OATP1A2 (SLCO1A2 gene) and OATP2B1 (SLCO2B1 gene) are responsible for transporting many medications, thyroid hormones, and estrogen metabolites into the brain. Studies on these transporters show that genetic variants impact how much of certain medications, including dopamine receptor agonists, make it to the brain. [ref][ref][ref]
The Large Neutral Amino Acid Transporter 1 (LAT1, or SLC7A5) transports essential amino acids and drugs like L-DOPA across the blood-brain barrier. Signaling molecules, like leptin, can move into the brain through endocytosis after binding to their receptors.[ref]
Tight Junctions:
The tight junctions between the endothelial cells in the tiny vessels in the brain rely on claudin-5 (CLDN5 gene) and occludin to maintain the integrity of the barrier. Animal studies show that a lack of claudin-5 (CLDN5) allows molecules that are smaller than 800 Da to pass through to the brain.[ref]
Breaking down the BBB:
Matrix metalloproteinases are a family of enzymes that can break down the extracellular matrix, which is important in remodeling and renewing blood vessels (and other tissues). In reference to the blood-brain barrier, an excess of MMP function can increase BBB leakiness.[ref]
More specifically, the matrix metalloproteinase called MMP9 is the primary one that breaks down the type IV collagen and fibrin in the BBB.[ref] (See the genotype report for MMP9 variants)
There are multiple ways that MMP9 levels are kept in balance. One that is important in the aging brain is that the correct APOE secretion from astrocytes is part of the way that MMP9 is suppressed. This directly ties together the maintenance of the BBB, APOE, and MMP9 in the pathology seen in neurodegenerative diseases.[ref]
Inflammation and BBB leakiness:
Chronically elevated inflammatory cytokines, including TNF-alpha and IL-1B, play a role in reducing barrier function directly through activating astrocytes. Some inflammatory cytokines can cross the BBB, but others, such as TGF-β1, can’t enter the brain. TNF-alpha crosses the BBB through receptor-mediated transport, meaning that the TNF receptor has to be present to move TNF-alpha into the brain. Keep in mind that the BBB is a two-way street, and inflammatory cytokines from the brain may be prevented from moving out in certain situations.[ref][ref]
Studies show that IL-1β, TNFα, and IL-6 break down tight junction proteins, including claudin-5 and occludin, between endothelial cells, significantly increasing permeability. [ref]
Related article: TNF alpha variants that increase inflammatory response
Fungal infection – Candida – as a cause of BBB dysfunction:
A 2025 study showed that a severe Candida albicans systemic infection can cross the blood-brain barrier in two different ways. First, the hypae can create a tunnel through the BBB; also, the presence of the fungus can increase inflammatory cytokines, causing the degradation of the tight junctions.[ref] Note that this is for a severe systemic Candida infection, which is usually only seen in someone who is severely immunocompromised.
Related article: Candida and genetic susceptibility
Which conditions are associated with BBB dysfunction?
Traumatic brain injury and stroke are acute conditions that can impair the BBB, but there are also a number of chronic conditions that a dysfunctional blood-brain barrier can impact.
Decreased BBB integrity can allow toxins or viruses into the brain, and it can also allow the body’s own inflammatory cytokines to flow into the central nervous system, increasing neuroinflammation, cognitive decline, and brain fog.
Let’s take a look at some of the research on conditions that involve a leaky blood-brain barrier.
ADHD and neurological disorders:
The CLDN5 gene encodes the claudin protein that maintains the blood-brain barrier tight junctions. A study in children and teens with ADHD (not on medications) showed that they had significantly lower CLDN5 levels than a matched control group.[ref]
Folate deficiency is implicated in several types of neurological disorders, including ASD and seizures. Folate transport across the BBB into the brain involves active endocytosis transport via folate receptor alpha (FOLR1 gene) and the reduced folate carrier (RFC).[ref]
Related article: FOLR1 genetic variants
Alzheimer’s and BBB dysfunction:
The BBB not only prevents toxins and viruses from reaching the brain, but it also can block substances from being removed from the brain. Amyloid-beta builds up in the brain in Alzheimer’s disease, and one reason is that BBB dysfunction can block the removal of amyloid beta.
Blood-brain barrier dysfunction is often an early event in Alzheimer’s disease, as shown on MRI imaging studies. The BBB dysfunction prevents the removal of amyloid beta from the brain. This is a vicious feedback loop where the amyloid deposits further damage the BBB.[ref][ref][ref]
Animal models of APOE E4 allele carriers show that the E4 allele increases MMP9, which breaks down the blood-brain barrier and impairs tight junctions. Intriguingly, removing APOE4 from the BBB region restored the blood-brain barrier integrity. This directly links the APOE E4 allele to BBB dysfunction and is likely playing a causal role in Alzheimer’s.[ref]
Related article: APOE type and Alzheimer’s risk (only read if you want to know it)
The blood-brain barrier in depression and schizophrenia:
BBB dysfunction is also part of major depressive disorder, PTSD, and schizophrenia.
In people with depression, several studies have shown markers of increased BBB permeability. Animal studies in models of depression show that there is a disruption of the tight junctions in the BBB epithelium. Stress is thought to cause a loss of claudin-5, and higher levels of circulating inflammatory cytokines, including TNF-alpha, also decrease claudin-5 expression, leading to BBB dysfunction.[ref] A recent preprint study showed that people with depression due to trauma, PTSD, or stress were likely to have higher methylation of CLDN5 (less gene expression), which increases BBB leakiness.[ref]
Related article: Inflammation, genetics, and depression
Recent studies show that a dysfunctional BBB plays a critical role in schizophrenia by potentially triggering a neuroinflammatory cascade. Patients with schizophrenia have altered tight junction protein expression, including low claudin-5 and higher levels of MMP-9. This disruption allows neurotoxic substances to reach the brain.[ref] A study on patients who had recently been diagnosed with schizophrenia found diagnostic signs of BBB dysruption in 18% of patients.[ref]
Related article: Schizophrenia genetic factors
Long Covid and brain fog:
Studies on people with long Covid and cognitive dysfunction show that the blood-brain barrier is affected. An MRI study showed persistent BBB dysfunction two years after Covid in participants who reported cognitive symptoms of long Covid. Another study used transcriptomics and found that: “sustained systemic inflammation and persistent localized BBB dysfunction is a key feature of long COVID-associated brain fog.”[ref][ref]
Prior studies show that increased BBB permeability is strongly associated with cognitive issues or brain fog.[ref][ref]
Related article: Brain fog – causes and your genes
Akathisia and transporting antipsychotic drugs out of the brain:
Akathisia is the feeling of intense restlessness and a need to move that often occurs after stopping certain types of psychiatric medications. It can cause pacing, rocking, and feeling like you’re jumping out of your skin. Researchers have traditionally thought of akathisia as involving overstimulation of certain brain regions and an imbalance of dopaminergic activation. However, newer studies are also showing that the blood-brain barrier may be involved.[ref]
The blood-brain barrier makes it hard for drugs to pass through to the brain, but it can also make it difficult for drugs to move back out of the brain. This brain –> blood direction is called efflux, and the ABC transporters are involved in moving drugs out of the brain.
Variants in ABCB1 increase the risk of akathisia in treatment with risperidone.[ref] Note that akathisia isn’t only due to the blood-brain barrier. Other genetic studies also point to the role of dopamine receptor variants.[ref]
Bacterial infections and gut-brain axis:
The body detects some bacterial pathogens by recognizing the lipopolysaccharide (LPS) on the bacterial membrane. LPS then causes a robust immune response, including in the blood-brain barrier. Researchers using animals showed that circulating LPS directly increases BBB permeability.[ref]
This ties to the health of your gut barrier to the gut-brain axis. A leaky gut barrier allows more bacterial exposure and LPS in the bloodstream, causing increased BBB permeability. Gut dysbiosis also increases LPS exposure in circulation, again leading to BBB dysfunction through altered tight junctions.[ref]
With this background information in mind, let’s take a look at how your genes influence the susceptibility to increased blood-brain barrier dysfunction.
Genotype report: Blood-Brain Barrier
Access this content:
An active subscription is required to access this content.
Lifehacks: Supporting the BBB
| Category | Recommendations | Evidence |
|---|---|---|
| Anti-Inflammatories | Resveratrol (500mg/day) Quercetin + Dasatinib (senolytic) Luteolin |
Reduces cytokines, preserves tight junctions |
| Nutrition | DHA/EPA (2g/day) Extra virgin olive oil (30ml/day) Carvacrol Normalize blood glucose |
Improves clearance post-trauma/AD |
| Probiotics | Lactobacillus and Bifidobacteria species | Reverses leakiness in PD models |
Decreasing inflammation:
Higher circulating inflammatory cytokines increase the permeability of the blood-brain barrier. Targeting inflammation with supplements such as resveratrol, curcumin, luteolin, or quercetin may help to reduce BBB dysfunction.[ref]
Resveratrol has specifically been studied in reference to reducing inflammatory cytokines and increasing the integrity of the blood-brain barrier.[ref]
Quercetin is a lipophilic molecule and can cross the blood-brain barrier. Studies on quercetin as a senolytic show that it, along with dasatinib, helps to preserve the BBB in aging animals.[ref]
Luteolin is another commonly used anti-inflammatory supplement. Studies in animals show that it helps to improve the expression of tight junction proteins in the BBB after strokes.[ref]
Nutritional support:
DHA and EPA:
Omega-3 fish oils with DHA and EPA may help to improve BBB function. Studies on damage after brain trauma show that increased DHA and EPA help to prevent the degeneration of tight junctions in the BBB.[ref]
Extra virgin olive oil:
A small clinical trial in mild Alzheimer’s patients showed that daily consumption of 30 mL of raw extra virgin olive oil decreases BBB dysfunction and improves cognition scores. The study notes that the consumption of extra virgin olive oil reduces the amyloid beta levels in the brain by increasing its clearance via the BBB. [ref] Note that this was a small study, and one of the authors is a shareholder in an olive oil company.
Caffeic acid phenethyl ester:
Studies show that caffeic acid increases the BBB integrity by increasing claudin-5 levels.[ref] Caffeic acid phenethyl ester is abundant in bee propolis.
Access this content:
An active subscription is required to access this content.
Related articles and Topics:
COMT: How to Optimize Your Supplements for Your COMT Genotype
Dopamine Synthesis SNPs: Genes, lifestyle, diet, and dopamine optimization