Key takeaways:
- Tyramine is a naturally occurring biogenic amine that can cause blood vessels to constrict and act as a norepinephrine mimetic.
- Excess tyramine can result in serious symptoms, such as heart palpitations, spiking blood pressure, stroke-like symptoms, nausea, gastrointestinal issues, migraines, cluster headaches, and brain fog.
- Genetic variants in key enzymes (MAOA, FMO3, CYP2D6, and DAO) impact how well you break down and eliminate tyramine.
- Medications, especially MAO-A inhibitors, can also significantly impact tyramine metabolism.
What is tyramine intolerance? Symptoms, foods, and breaking it down
Tyramine intolerance is a sensitivity where eating foods high in tyramine (like aged cheese, cured meats, or leftovers) triggers symptoms such as severe migraines, blood pressure spikes, or gut problems because your body cannot break tyramine down efficiently.
Tyramine is a biogenic amine that is derived from the amino acid tyrosine when it is broken down by bacteria. Higher tyramine levels cause the release of norepinephrine in the body, which then increases blood pressure. High tyramine content is often found in aged, fermented, or slightly spoiled foods.
Genetic variants in the genes related to tyramine metabolism cause a large inter-individual variability in the response to tyramine.[ref]
High tyramine levels in meals can trigger a hypertensive crisis, commonly known as the cheese effect from tyramine. This is usually associated with taking a drug type called an MAO-A inhibitor (MAOI), a class of drugs that includes phenelzine, tranylcypromine, and isocarboxazid. People on an MAOI are cautioned by their doctor about the dietary interactions, such as with aged cheeses. The hypertensive crisis is caused by too much tyramine, causing a sudden blood pressure increase and leading to other symptoms.
In addition to medication interactions with MAOIs, genetic variants play a role in how well the body handles tyramine. I’ll start with some background on tyramine and then explain the genetic variants that can decrease your ability to metabolize and eliminate tyramine.
What is tyramine, and why does it cause symptoms?
Tyramine is a biogenic amine, which refers to its chemical structure with nitrogen at its base. Other biogenic amines include histamine, spermidine, dopamine, serotonin, epinephrine, and norepinephrine, which are all amines that we create naturally. Structurally, tyramine is a monoamine, similar to norepinephrine, dopamine, and serotonin.
It is naturally found at trace levels in the human body. Tyramine, even in low amounts, causes the release of catecholamine neurotransmitters. It can cross the blood-brain barrier and act as a neuromodulator in the brain. It can also take the place of norepinephrine, binding to the receptors that cause blood vessel constriction.[ref][ref]
Bacteria convert the amino acid tyrosine into tyramine, and fermented foods, aged cheeses, and foods close to spoiling can have very high amounts of tyrosine. This is where the term ‘cheese effect‘ comes into play, because researchers first discovered the hypertensive effects of tyrosine when people on MAOI drugs ate aged cheeses. [ref]
In addition, certain gut microbes can also produce tyramine, adding to the body’s overall tyramine levels. Tyramine is absorbed in the intestines and transported by the OCT1 transporter.
How does the body get rid of tyramine?
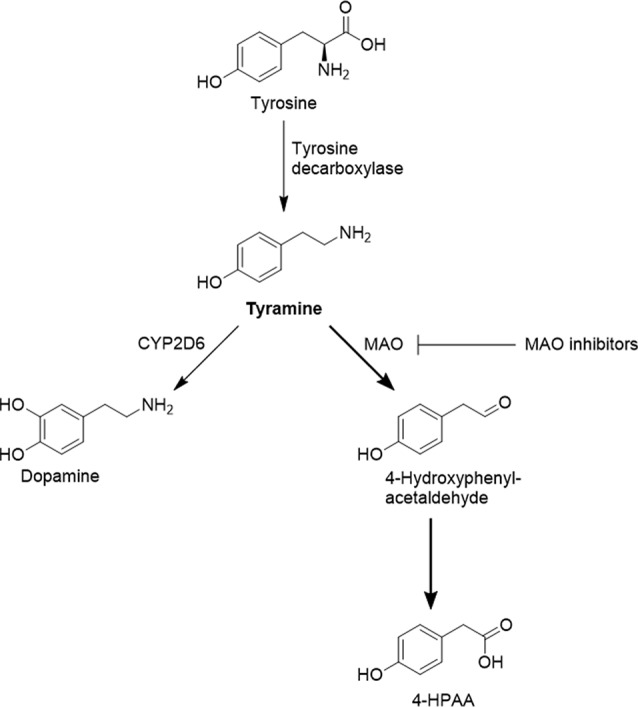
In the intestines, tyramine is absorbed from foods and from gut microbial production. From there, it enters the circulation and is then broken down primarily in the liver. Tyramine is mainly broken down (metabolized) in the body using the MAO-A (monoamine oxidase) enzyme, but three other enzymes, CYP2D6, FMO3, and DAO, can also act on tyramine.
| Enzyme | Role |
|---|---|
| MAO-A | Primary enzyme, breaks down neurotransmitters; inhibited by MAOIs, increasing risk |
| FMO3 | Supports tyramine breakdown |
| CYP2D6 | Liver enzyme, detoxifies various compounds, including tyramine |
| DAO | Intestinal enzyme, breaks down histamine in the intestines along with other biogenic amines (including tyramine) |
The MAO-A enzyme is the primary way the body breaks down tyramine. It also metabolizes (breaks down) several neurotransmitters, including dopamine. Thus, inhibiting MAO-A is one way to increase dopamine levels. Drugs that act as MAO-A inhibitors (MAOIs) can be used as antidepressants, although they usually aren’t the first drug choice due to the interactions with tyramine in foods. In addition to drug interactions, genetic variants in the MAOA gene affect the metabolism of tyramine and the blood pressure response.[ref]
CYP2D6 is a detoxification enzyme produced primarily in the liver and in the brain. It breaks down toxins, medications, and some substances produced in the body, such as serotonin. In tyramine metabolism, the CYP2D6 enzyme acts as a catalyst to convert tyramine to dopamine.[ref]
FMO3 (flavin-containing monooxygenase 3) is another enzyme produced in the liver that can metabolize tyramine. Specifically, FMO3 oxidizes tyramine, converting it into trans-oxime.[ref]
The DAO (diamine oxidase) enzyme is responsible primarily for breaking down histamine in foods. Recent studies show that it can also be a backup route for metabolizing other biogenic amines, including tyramine.[ref] Genetic variants in the AOC1 gene, which encodes the DAO enzyme, are also found in histamine intolerance. Some of the symptoms of histamine intolerance, such as gastrointestinal issues and headaches, overlap with tyramine intolerance, making it difficult to distinguish the two conditions.
Tyramine reactions:
Tyramine is similar to norepinephrine in structure, and it can activate norepinephrine receptors at high levels.
Tyramine intolerance symptoms include:
- migraines
- BP spikes
- gastrointestinal issues
- brain fog
- heart palpitations
Let’s take a look at some of these effects in detail:
Tyramine causes migraines or cluster headaches:
Research shows that for people susceptible to migraines, a list of foods high in tyramine often corresponds to their list of ‘triggers’. Many people with either cluster headaches or migraines don’t break down tyramine well.[ref]
Why headaches from tyramine? Researchers think that vasoconstriction triggered by high tyramine levels initiates the migraine.[ref][ref]
Related article: Migraines, genetic causes
Blood pressure spike:
If you get too much tyramine due to eating foods high in tyramine and not breaking down the tyramine (e.g., when taking an MAO-A inhibitor), it can throw your body into a hypertensive crisis, raising systolic blood pressure by 30 mmHg or more.
This is called the ‘tyramine pressor response’. Tyramine takes the place of other neurotransmitters, triggering the body to release a bunch of norepinephrine, constricting blood vessels, and raising blood pressure. Tyramine can also take the place of norepinephrine in activating receptors.[ref]
You may wonder why everyone doesn’t have a stroke or heart attack after eating a salami and aged cheese sandwich on sourdough bread. There are a couple of reasons for this:
- First, most people break down tyramine fairly well. There are three different enzyme pathways to take care of it.
- Second, repeated exposure to tyramine will decrease the tyramine pressor response. It’s the change from typically not eating foods high in tyramine to suddenly chowing down on them that can cause a response. For instance, eating a healthy diet full of fresh foods — and then hitting the holiday buffet and having salami, cheese, and olives, chased with a glass of red wine.
Gut activation:
In addition to blood vessel constriction, when tyramine levels are high, it can activate the ADRA2A (alpha-2A adrenergic receptor), which is a norepinephrine receptor that regulates insulin secretion, anxiety, sympathetic neurons, and also neurons in the gut. In the intestines, certain gut bacteria can produce tyramine, and this can activate ADRA2A. In an animal model of IBD (Crohn’s, ulcerative colitis), it was recently shown that this tyramine –> ADRA2A activation pathway suppresses the intestinal stem cells that can repair and maintain the gut barrier.[ref]
Related article: Inflammatory Bowel Diseases
Fatty liver:
Tyramine from the gut microbiome may also play a role in fatty liver disease (NAFLD). A study involving children with obesity showed that their gut microbiome had more Enterococcus faecium, which produces tyramine. The increased tyramine activated PPAR-gamma, leading to lipid accumulation and NAFLD.[ref]
Related article: Fatty liver disease (NAFLD, MAFLD)
Notable/Interesting Points:
- Tyramine is chemically similar to amphetamines but does not have the same effects.[ref]
- Florida banned tyramine in 2012 as a Schedule I drug. (Does this make aged cheese illegal in Florida?)
Which foods are high in tyramine?
Foods high in tyramine include:
| High Sources | Medium Sources |
|---|---|
| Aged/smoked meats (salami, bacon, jerky) | Olives |
| Aged cheeses (cheddar, Swiss, Parmesan, feta) | Chocolate |
| Sourdough, homemade yeast bread | Snow peas, edamame |
| Marmite, fermented veggies, dried fruits | Avocados, bananas |
| Some beers/wines (esp. unpasteurized) | Pineapple, eggplant |
| Figs, yogurt, sour cream | |
| Peanuts, Brazil nuts | |
| Fava beans |
Is it histamine or tyramine intolerance?
Many foods that are high in tyramine are also high in histamine. You may find it difficult to know whether you’re reacting to histamine or tyramine in foods. Read this histamine intolerance article to learn about genetic susceptibility, similarities, and symptom differences.
One significant difference in tyramine intolerance vs. histamine intolerance is the hypertensive crisis. A spike in blood pressure is associated with high tyramine levels and not histamine intolerance.
Tyramine Metabolism Genotype Report
This is a SNP-based nutrigenomics framework to help you identify if you are likely to have reduced enzyme activity for tyramine metabolism. The variants below have been studied in reference to their impact on enzyme activity in the biochemical pathways that metabolize tyramine.
Reduced enzyme activity in just one gene is not likely to cause significant problems with high tyramine foods, since there are multiple pathways for the metabolism of tyramine. However, reduced activity in a couple of the genes theoretically could cause problems with tyramine metabolism. Keep in mind that tyramine intolerance depends on your intake of high tyramine foods, your gut microbiome, and any medication interactions.
Tyramine from food is mainly broken down in the liver using the enzymes MAOA, FMO3, and CYP2D6.[ref] In addition, the DAO enzyme produced in the intestines to break down histamine can also metabolize tyramine and other biogenic amines.
MAO-A gene: Encodes monoamine oxidase A (MAOA) enzyme, which breaks down tyramine, serotonin, dopamine, epinephrine, and norepinephrine. It is located on the X chromosome, so males will only have one copy of the gene.
Related article: MAO-A and MAO-B: Neurotransmitter levels, genetics, and studies
Access this content:
An active subscription is required to access this content.
Lifehacks: Natural solutions for tyramine intolerance
Let’s take a look at how to support tyramine metabolism, which foods to avoid, and which supplements are likely to impair tyramine breakdown.
Supporting tyramine metabolism:
Riboflavin for tyramine intolerance:
Vitamin B2 (riboflavin) is important in two ways for the breakdown of tyramine.
- Riboflavin is a cofactor for the MAO-A enzyme.[ref]
- Riboflavin is necessary for FMO3 function.[ref][ref]
This may be one reason that riboflavin works to prevent migraines in some people.
Make sure you get enough riboflavin via your diet or consider supplementing with riboflavin. The RDA for riboflavin is 1.3 mg daily for adult men and 1.1 mg daily for adult women. Foods high in riboflavin include milk, yogurt, cheese, eggs, meats, and green leafy vegetables.
Related article: Riboflavin genetic variants
NAD+ for MAO-A support:
MAO-A is also dependent on NAD+ levels, and NAD+ levels decline with age. To support NAD+, consider NMN or NR if you are older.
Related article: NAD+, NR, and NMN
DAO enzyme supplements:
Diamine oxidase is the enzyme that breaks down histamine and tyramine in the intestines. DAO supplements are available and may be helpful for someone with DAO variants (AOC1 gene).
Related article: DAO Enzyme Supplement Research
Avoiding high tyramine foods:
Access this content:
An active subscription is required to access this content.
Related Articles and Topics:
Trimethylaminuria: FMO3 mutations that cause malodorous body odor
References:
“Avoid the Combination of High-Tyramine Foods and MAOIs.” Mayo Clinic, https://www.mayoclinic.org/diseases-conditions/depression/expert-answers/maois/faq-20058035. Accessed 16 Nov. 2025.
Barger, G., and G. S. Walpole. “Isolation of the Pressor Principles of Putrid Meat.” The Journal of Physiology, vol. 38, no. 4, Mar. 1909, pp. 343–52. PubMed Central, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1533642/.
Bushueva, Olga, et al. “The Flavin-Containing Monooxygenase 3 Gene and Essential Hypertension: The Joint Effect of Polymorphism E158K and Cigarette Smoking on Disease Susceptibility.” International Journal of Hypertension, vol. 2014, Aug. 2014, p. e712169. www.hindawi.com, https://doi.org/10.1155/2014/712169.
D’Andrea, G., et al. “Biochemistry of Neuromodulation in Primary Headaches: Focus on Anomalies of Tyrosine Metabolism.” Neurological Sciences, vol. 28, no. 2, May 2007, pp. S94–96. Springer Link, https://doi.org/10.1007/s10072-007-0758-4.
Hotamisligil, G. S., and X. O. Breakefield. “Human Monoamine Oxidase A Gene Determines Levels of Enzyme Activity.” American Journal of Human Genetics, vol. 49, no. 2, Aug. 1991, pp. 383–92.
How a Migraine Happens. 26 Nov. 2019, https://www.hopkinsmedicine.org/health/conditions-and-diseases/headache/how-a-migraine-happens.
Kashyap, A. S., and Surekha Kashyap. “Fish Odour Syndrome.” Postgraduate Medical Journal, vol. 76, no. 895, May 2000, pp. 318–318. pmj.bmj.com, https://doi.org/10.1136/pmj.76.895.318a.
Koukouritaki, Sevasti B., et al. “Discovery of Novel Flavin-Containing Monooxygenase 3 (FMO3) Single Nucleotide Polymorphisms and Functional Analysis of Upstream Haplotype Variants.” Molecular Pharmacology, vol. 68, no. 2, Aug. 2005, pp. 383–92. PubMed, https://doi.org/10.1124/mol.105.012062.
Li, Chaoliang, et al. “Enterococcus-Derived Tyramine Hijacks α2A-Adrenergic Receptor in Intestinal Stem Cells to Exacerbate Colitis.” Cell Host & Microbe, vol. 32, no. 6, June 2024, pp. 950-963.e8. PubMed, https://doi.org/10.1016/j.chom.2024.04.020.
Ma, Peng, et al. “Gut Microbiota Metabolite Tyramine Ameliorates High-Fat Diet-Induced Insulin Resistance via Increased Ca2+ Signaling.” The EMBO Journal, vol. 43, no. 16, Aug. 2024, pp. 3466–93. PubMed, https://doi.org/10.1038/s44318-024-00162-w.
Manning, Nigel J., et al. “Riboflavin-Responsive Trimethylaminuria in a Patient with Homocystinuria on Betaine Therapy.” JIMD Reports, vol. 5, 2012, pp. 71–75. PubMed, https://doi.org/10.1007/8904_2011_99.
Medori MC, et al. (2023). Nutrigenomics: SNPs Correlated to Food Preferences and Susceptibilities. La Clinica Terapeutica, 174(Suppl 2):214–226. DOI: 10.7417/CT.2023.2490. PMID: 37994767
Niwa, Toshiro, et al. “Human Liver Enzymes Responsible for Metabolic Elimination of Tyramine; a Vasopressor Agent from Daily Food.” Drug Metabolism Letters, vol. 5, no. 3, Aug. 2011, pp. 216–19. PubMed, https://doi.org/10.2174/187231211796905026.
NM_006894.5(FMO3):C.913G>T (p.Glu305Ter) AND Trimethylaminuria – ClinVar – NCBI. https://www.ncbi.nlm.nih.gov/clinvar/RCV000017697.30/. Accessed 16 Nov. 2022.
NM_001002294.3(FMO3):C.589_590TG[1] (p.Cys197_Asp198delinsTer) AND Trimethylaminuria – ClinVar – NCBI. https://www.ncbi.nlm.nih.gov/clinvar/RCV000490504.1/. Accessed 16 Nov. 2022.
Rafehi, Muhammad, et al. “Highly Variable Pharmacokinetics of Tyramine in Humans and Polymorphisms in OCT1, CYP2D6, and MAO-A.” Frontiers in Pharmacology, vol. 10, Oct. 2019, p. 1297. PubMed Central, https://doi.org/10.3389/fphar.2019.01297.
Sathyanarayana Rao, T. S., and Vikram K. Yeragani. “Hypertensive Crisis and Cheese.” Indian Journal of Psychiatry, vol. 51, no. 1, 2009, pp. 65–66. PubMed Central, https://doi.org/10.4103/0019-5545.44910.
Sánchez-Pérez, Sònia, et al. “The Rate of Histamine Degradation by Diamine Oxidase Is Compromised by Other Biogenic Amines.” Frontiers in Nutrition, vol. 9, May 2022, p. 897028. PubMed Central, https://doi.org/10.3389/fnut.2022.897028.
tammy-lrome. “Low-Tyramine Diet Essentials.” Migraine.com, https://migraine.com/blog/low-tyramine-diet-essentials.
Walker, S. E., et al. “Tyramine Content of Previously Restricted Foods in Monoamine Oxidase Inhibitor Diets.” Journal of Clinical Psychopharmacology, vol. 16, no. 5, Oct. 1996, pp. 383–88. PubMed, https://doi.org/10.1097/00004714-199610000-00007.
Xu, Meijuan, et al. “Genetic and Nongenetic Factors Associated with Protein Abundance of Flavin-Containing Monooxygenase 3 in Human Liver.” The Journal of Pharmacology and Experimental Therapeutics, vol. 363, no. 2, Nov. 2017, pp. 265–74. PubMed, https://doi.org/10.1124/jpet.117.243113.
Xu, Xiaohui, et al. “Association Study between the Monoamine Oxidase A Gene and Attention Deficit Hyperactivity Disorder in Taiwanese Samples.” BMC Psychiatry, vol. 7, Feb. 2007, p. 10. PubMed, https://doi.org/10.1186/1471-244X-7-10.