Key takeaways:
~ Serotonin is a neurotransmitter in the brain and the peripheral nervous system.
~ Serotonin is also made in the gut and is important in the immune system and gut health.
~ Genetic variants impact how the serotonin system works, and diet, supplements, and lifestyle can impact serotonin levels.
What does serotonin do?
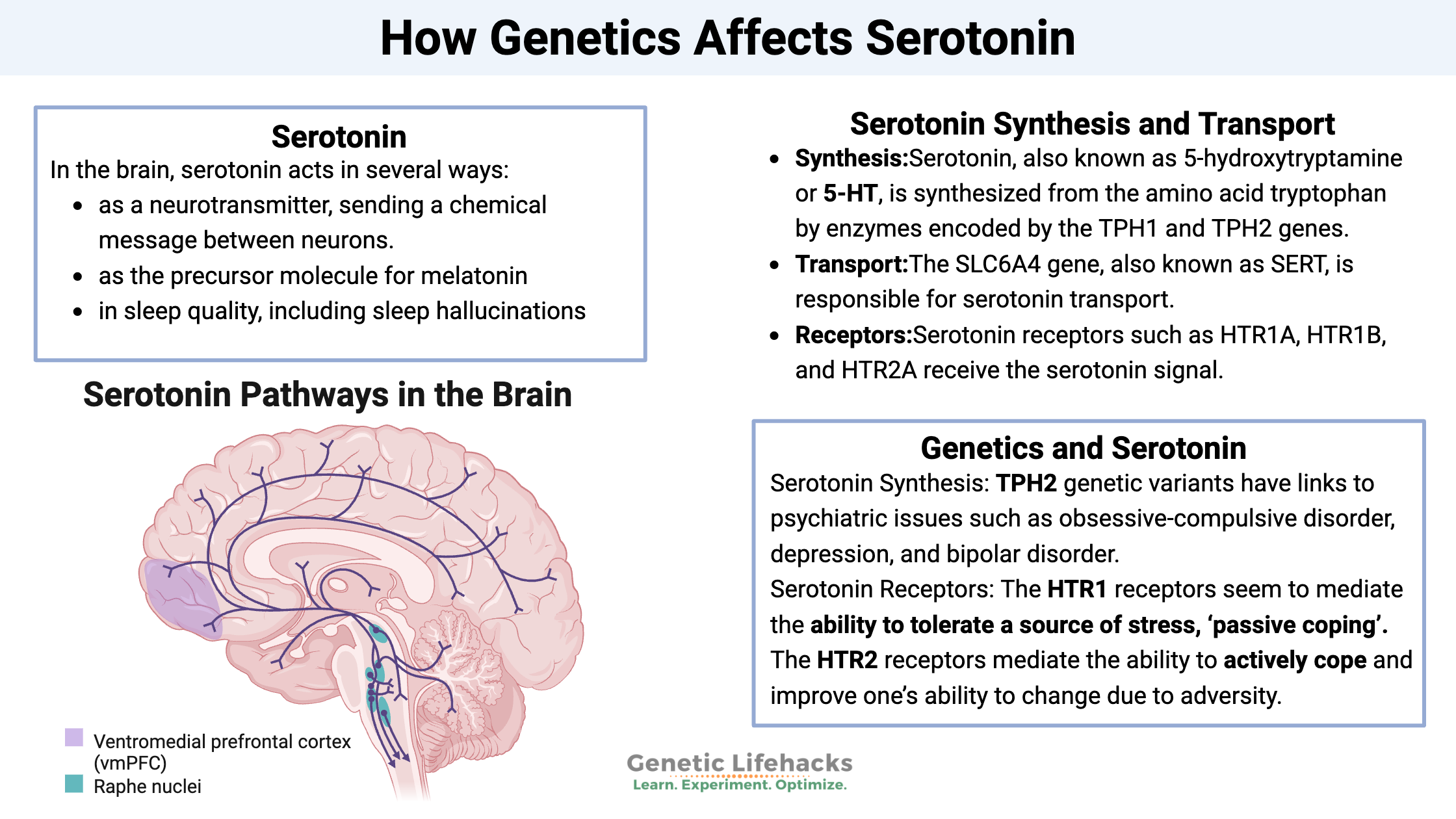
In the brain, serotonin acts in several ways:
- as a neurotransmitter, sending a chemical message between neurons.
- as the precursor molecule for melatonin
- in sleep quality, including sleep hallucinations[ref][ref]
But there is more to serotonin than just its impact on the brain.
About 90% of serotonin is made in the gut and helps to regulate motility.[ref] Serotonin also regulates other functions such as bone mass, cardiovascular health, the endocrine system, and appetite.
Serotonin is also important in energy metabolism, heart rate, cell growth, and immunity.[ref]
| System/Function | Role of Serotonin |
|---|---|
| Brain | Mood, sleep, melatonin precursor |
| Gut | Motility, majority of serotonin made |
| Immune system | Modulates inflammation |
| Other | Bone mass, cardiovascular, endocrine |
Serotonin and Mental Health
Some researchers believe that imbalances in serotonin may play a role in depression or anxiety. Common antidepressants, including SSRIs (selective serotonin reuptake inhibitors), are prescribed to elevate serotonin levels in the brain. However, the method through which they work is still not completely understood.[ref]
Another link between serotonin and depression is that serotonin modulates immune function.[ref] This ties into research showing that increased inflammation is one root cause of major depressive disorder.
Related article: Depression, chronic inflammation, and genetic susceptibility
Recent animal research shows that one reason that SSRIs may not work for everyone is due to increased inflammation. The study showed that in inflammatory situations, histamine is upregulated, and SSRIs act in off-target actions on histamine instead of increasing serotonin. In this study, decreasing histamine levels increased SSRI effectiveness.[ref]
Related article: Histamine intolerance genes
Serotonin Synthesis and Transport:
Like most signaling molecules and neurotransmitters, serotonin first needs to be created (synthesized), then it needs to be transported, and finally, the signal needs to be received by a cellular receptor.
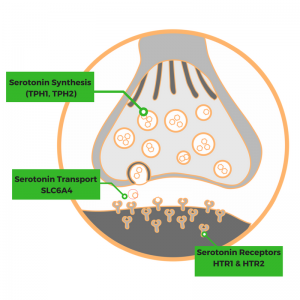
Synthesis:
Serotonin, also known as 5-hydroxytryptamine or 5-HT, is synthesized from the amino acid tryptophan by enzymes encoded by the TPH1 and TPH2 genes.
Transport:
The SLC6A4 gene, also known as SERT, is responsible for serotonin transport.
Receptors:
Serotonin receptors such as HTR1A, HTR1B, and HTR2A receive the serotonin signal.
All of these work in concert: from the creation of serotonin from amino acids to the transport of serotonin to the receptors that are necessary to receive this chemical messenger.
Serotonin Syndrome: Too much serotonin
Ultimately, balance is the key to serotonin. An excess of serotonin can result in serotonin syndrome. Symptoms include restlessness, confusion, shivering, diarrhea, and, potentially, death.[ref] Serotonin syndrome is usually caused by drugs such as MAOIs or SSRIs that affect the rate of serotonin breakdown.[ref]
Genetics and Serotonin:
Genes play a role in how your cells synthesize, transport, and receive the serotonin signal. (You’ll find your genotypes for these genetic variants in the Genotype report below.)
Serotonin Synthesis: Tryptophan Hydroxylase (TPH1 and TPH2)
Tryptophan hydroxylase is an enzyme that catalyzes the reaction that produces serotonin from the amino acid tryptophan. Iron is a cofactor, and BH4 is also used in the reaction.
There are two genes that code for tryptophan hydroxylase:
- TPH1 is found mainly in the gut, skin, and pineal gland.
- TPH2 works in the central nervous system.
Related article: How tryptophan converts to serotonin or kynurenine
Several TPH2 genetic variants have links to psychiatric issues such as obsessive-compulsive disorder, depression, and bipolar disorder. These variants affect the production rate of serotonin in the brain.
Serotonin Receptors: HTR1A, HTR1B, HTR2A
While there is still debate among researchers on this topic, one recent paper explains that the function of the brain’s serotonin receptors is to moderate stress and anxiety through patience and coping.
- The HTR1 receptors seem to mediate the ability to tolerate a source of stress, ‘passive coping’.
- The HTR2 receptors mediate the ability to actively cope and improve one’s ability to change due to adversity.
Serotonin Transporter: 5-HTTLPR Short and Long
SLC6A4 is the gene that encodes the serotonin transporter. You will find it as SERT or 5-HTT in some of the research. The 5-HTTLPR variant is a variable number tandem repeat. This just means there is a short version of the gene and a long version – due to repeated parts of the gene.
A lot of researchers have studied the 5-HTTLPR short/short and long/long forms. Initial studies in the ’90s and early 2000s found that those with the short version of the gene were more prone to depression due to stressful events. Here is a nice article summarizing the research that has been done on this gene: Controversial Gene-Depression Link Confirmed in New Study.
A recent study may explain some of the contradictory results from previous studies.[ref] The researchers found that people who carried two copies of the long allele were more affected by environmental influences on mood (e.g., good or bad life events). Thus, people who carried the long/long genotype were more likely to have a positive mood in a positive environment, but they were also more negative when bad things happened.
Serotonin plays a major role in the gut, and IBS patients with a short allele had worse symptoms than those with a long/long version of this gene.[ref]
Related article: IBS genes
The short/short genotype also has ties to an increased risk of gastrointestinal intolerance of metformin.[ref]
| Gene | Function | Where It Acts | Notable Variants & Effects |
|---|---|---|---|
| TPH1 | Serotonin synthesis | Gut, skin, pineal gland | – |
| TPH2 | Serotonin synthesis | Central nervous system | Linked to psychiatric conditions |
| SLC6A4 | Serotonin transporter (SERT) | Brain, gut | 5-HTTLPR short/long: affects mood, IBS |
| HTR1A/B | Serotonin receptor (stress coping) | Brain | Mediate passive coping |
| HTR2A | Serotonin receptor (active coping) | Brain | Mediate active coping |
Serotonin Genotype Report:
Access this content:
An active subscription is required to access this content.
Lifehacks for Serotonin:
Below you will find research-supported ways of affecting your serotonin levels. If you need psychiatric help, please be sure to contact a healthcare provider!
Sunshine, exercise, and diet: Get outside, be active, and eat well
While your genes have an effect on serotonin levels in the body, there are also several environmental factors that also influence serotonin production.
- Sunlight exposure:
There is a correlation between higher serotonin levels and exposure to bright light or sunlight.[ref] - Move more, exercise:
Physical activity may also increase serotonin levels. Eating foods high in tryptophan may also increase serotonin levels, but it is hard to know how much of an effect it has on serotonin levels in the brain.[ref]
Gut health: Serotonin production in the gut microbiome
Access this content:
An active subscription is required to access this content.
Related Articles and Topics:
References: