Key Takeaways:
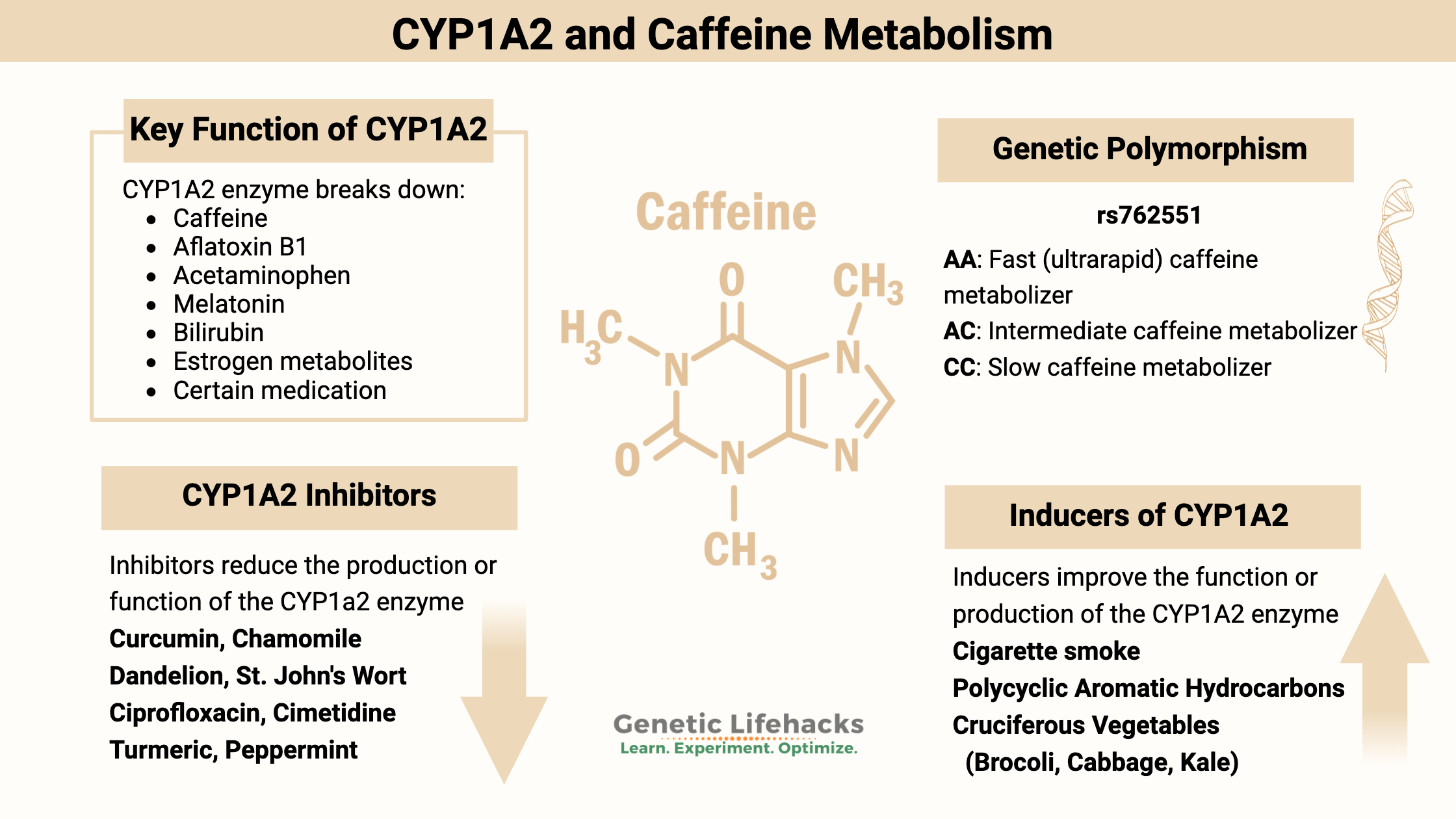
~ CYP1A2 is a phase I detoxification enzyme that breaks down caffeine as well as several important toxins, such as aflatoxin B1 from mold.
~ CYP1A2 also plays a role in estrogen metabolism and melatonin metabolism.
~ Common genetic variants in CYP1A2 influence whether you are a fast or slow metabolizer of caffeine and other CYP1A2 substrates.
Members will see their genotype report below, plus additional solutions in the Lifehacks section. Join today.
CYP1A2 Function: Caffeine Metabolism and More
The CYP family of genes codes for enzymes that are used by the body to break down and get rid of things like toxins, pollutants, drugs, and substances our body naturally makes. Genetic variants in the CYP genes impact how quickly we break down various drugs and other toxins, and understanding your genetic polymorphisms (variants) can shed light on how your body reacts to things.
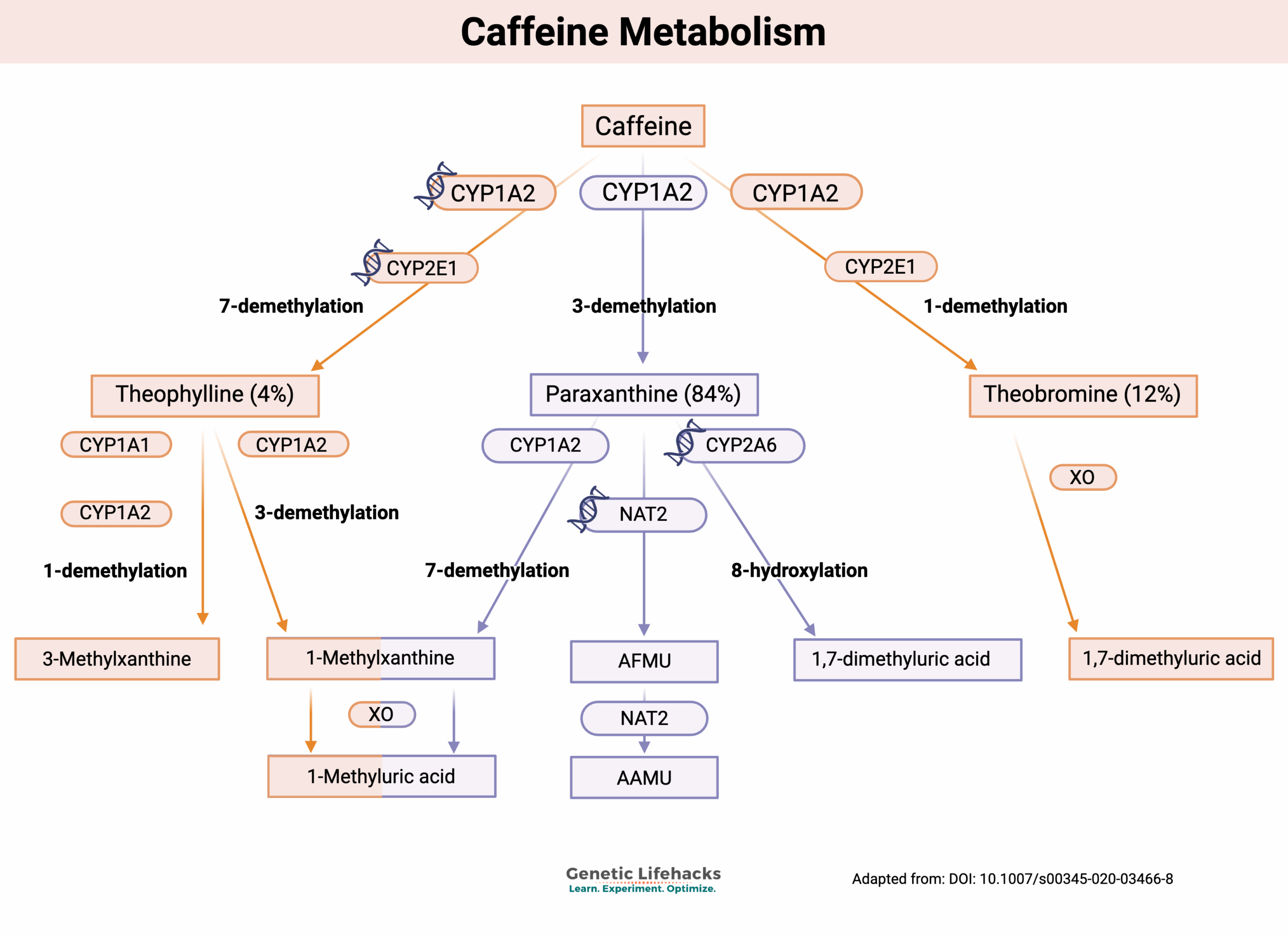
The function of the CYP1A2 enzyme is to break down certain substances to make them more easily excreted from the body. Specifically, the CYP1A2 enzyme is involved in the metabolism (breakdown) of caffeine and aflatoxin B1, a mold toxin found on grains and peanuts.[ref]
In addition, CYP1A2 also breaks down endogenous substances in the body, such as:
- melatonin
- bilirubin
- estrogens
Related article: Estrogen metabolism (including role of CYP1A2) and Gilbert’s Syndrome
Medications:
CYP1A2 also breaks down several prescription medications (substrates). Common medications for which CYP1A2 is involved in metabolism include:[ref][ref][ref]
- clozapine
- olanzapine
- theophylline
- tizanidine
- paroxetine
- escitalopram
However, many medications are metabolized by multiple CYP enzymes, so genetic variants in CYP1A2 alone may not accurately predict your response to a medication.
Substrates, Inducers, and Inhibitors:
- When it comes to the CYP450 enzymes, substrates are the substances that the enzyme acts on to break it down. Caffeine would be an example of a substrate of CYP1A2.
- Other substances, called inducers, cause the body to produce more of the enzyme. Cigarette smoke is an example of an inducer.
- Inhibitors are substances that inhibit the enzyme from being produced or from working normally.
Genetic variants interact with medications as well as other substances (such as caffeine) that are metabolized by the same enzyme.[ref] For example, someone with a slow CYP1A2 genotype may find that taking an inhibitor of CYP1A2 at the same time as drinking a caffeinated beverage causes the caffeine to remain in their system longer.
There is a list of drugs, inducers, and inhibitors of CYP1A2 on Wikipedia.
What speeds up CYP1A2 (inducers)?
The polycyclic aromatic hydrocarbons (PAHs) found in cigarette smoke upregulate or increase the expression of CYP1A2. PAHs are also produced in incomplete combustion, such as wood fires, vehicle exhaust, or coal burning.
The largest source of PAHs is due to cigarette smoking or heavy marijuana smoking.[ref]
- Cigarette smoking may cause a faster clearance of some drugs that are metabolized through CYP1A2.
- Smoking may also make you clear out caffeine faster.
For example, smokers who take duloxetine may end up with lower levels of the drug in their system because cigarette smoke speeds up CYP1A2.[ref]
CYP1A2 is also induced (activated) by cruciferous vegetables such as cabbage, cauliflower, and broccoli.[ref] This is one reason why cruciferous vegetables may be beneficial for clearing out estrogen metabolites, through inducing more CYP1A2.
Related article: Estrogen metabolism
Phenytoin, an antiseizure medication, is also a moderate inducer of CYP1A2.[ref]
Which supplements and drugs inhibit CYP1A2?
CYP1A2 is inhibited, at least partially, by the following natural supplements:[ref][ref][ref]
- Curcumin and turmeric
- Peppermint
- Chamomile
- Dandelion
- St. John’s wort
Fluvoxamine is an SSRI that is also a strong CYP1A2 inhibitor.[ref] Ciprofloxacin (antibiotic), methoxsalen, and oral contraceptives are considered moderate CYP1A2 inhibitors.[ref]
If you take an inhibitor supplement along with drinking a caffeinated drink, you may find that the effects of caffeine last longer.
CYP1A2 Gene: Ultrarapid metabolizers vs. decreased activity
In looking at CYP1A2, there are several polymorphisms, or SNPs, that either increase the activity or decrease the activity of this enzyme.
People who have the A/A genotype for rs762551 are rapid or ultrarapid metabolizers. This means that they will break down or metabolize substances such as caffeine more rapidly. Caffeine is cleared out more quickly and does not affect an ultrarapid metabolizer for as long. Unsurprisingly, ultrarapid metabolizers also tend to drink more coffee, on average.[ref]
The rs762551 C/C genotype is linked to decreased CYP1A2 enzyme activity. People with this genotype will break down caffeine more slowly and may find that it bothers their sleep at night. You’ll see your genotypes below in the genotype report section.
What are the symptoms of slow or fast CYP1A2?
Well, it depends on what substance you are breaking down.
For example, CYP 1A2 metabolizes some pro-carcinogens from tobacco smoke into carcinogens. It also helps to turn aflatoxins (molds found in grains) into active compounds involved in liver cancer. Once CYP1A2 converts the original substance into the carcinogenic metabolite, the body must eliminate it. Genetic variants can also impact how quickly the second phase of detoxification works.
Thus, the rate at which CYP1A2 metabolizes certain toxins affects the risk of certain cancers in conjunction with how well Phase II detoxification moves out the metabolites.
A slow or reduced function isn’t always bad. For example, slow or inactive CYP1A2 is thought to decrease the risk of liver toxicity from aflatoxin B.[ref] This is because CYP1A2 turns the pro-carcinogenic molecules into carcinogens, which then have to be removed from the body.
Viral infections, Covid, and inflammation decrease CYP1A2:
Acute inflammation can decrease the production of CYP enzymes. This could be important in the way that the body metabolizes medications during an infection. Studies show that acutely elevated inflammatory cytokines can dramatically reduce CYP1A2 levels.[ref]
Viral infections can also alter CYP enzyme levels. Studies show that CYP1A2 enzyme activity is decreased by over 50% during a SARS-CoV-2 infection.[ref]
If you are on a medication that is metabolized using the CYP1A2 enzyme, you may find that a viral infection or acute inflammation will alter your response to medications. For example, there are reports of toxicity for clozapine and theophylline after the onset of respiratory infections.[ref]
CYP1A2 Genotype report:
One of the fun things to find out about your CYP1A2 genes is whether you are a fast or slow metabolizer of caffeine. This first SNP (polymorphism) is very well studied for the speed of caffeine metabolism.
Access this content:
An active subscription is required to access this content.
Lifehacks for CYP1A2
Your genetic variants are estimated to determine about 75% of your CYP1A2 enzyme activity, with food, supplements, and smoking impacting about 25% of the enzyme activity level.[ref]
Thus, if you are taking a drug, such as clozapine, that is metabolized by CYP1A2, you should look at both your genes and interactions with smoking, especially if combining that with a supplement that decreases CYP1A2 activity.
Which drugs are metabolized by CYP1A2?
Drugs that are metabolized by CYP1A2 include: [ref][ref]
- caffeine
- clozapine
- fluvoxamine
- melatonin (endogenous and exogenous)
- olanzapine
- ramelteon
- tacrine
- theophylline
- zolmitriptan
CYP1A2 inhibitors:
Curcumin is an inhibitor of CYP1A2 in humans and in animals. As I mentioned above, aflatoxin B is converted by CYP1A2 into a metabolite that is carcinogenic. Thus, inhibiting CYP1A2 with curcumin slows down the conversion of aflatoxin B into the carcinogen, which is helpful if you have slow phase II detoxification.
A recent animal study found that curcumin prevented liver damage from aflatoxin B exposure. A potent carcinogen, aflatoxin B is a toxin produced by mold (Aspergillus) and is sometimes found in peanuts, corn, and other grains. Curcumin can be taken as a supplement and is also found in the spice, turmeric.
Ciproflaxin, a commonly prescribed antibiotic, is also an inhibitor of CYP1A2.[ref]
A commonly used antihistamine, cimetidine (brand name Tagamet), is also a CYP1A2 inhibitor.[ref]
Keep in mind that your caffeine metabolism may be altered when taking a CYP1A2 inhibitor. In other words, if you are normally a fast metabolizer and drink coffee or tea with dinner, you may find yourself having problems sleeping if you pair caffeine with a CYP1A2 inhibitor like cimetidine, curcumin, or ciprofloxacin.
Melatonin supplements and CYP1A2:
Access this content:
An active subscription is required to access this content.
Related Articles and Topics:
CYP2D6: Medication Interactions, Natural Inhibitors, and Anxiety Traits
References: