Key takeaways:
~ The CYP2C19 gene is important in how your body responds to medications and breaks down toxins.
~ Variants in the CYP2C19 gene impact your response to medications such as omeprazole, clopidogrel, diazepam, and certain SSRIs.
Members will see their genotype report below and the solutions in the Lifehacks section. Consider joining today.
CYP2C19: Important for SSRIs, blood thinners
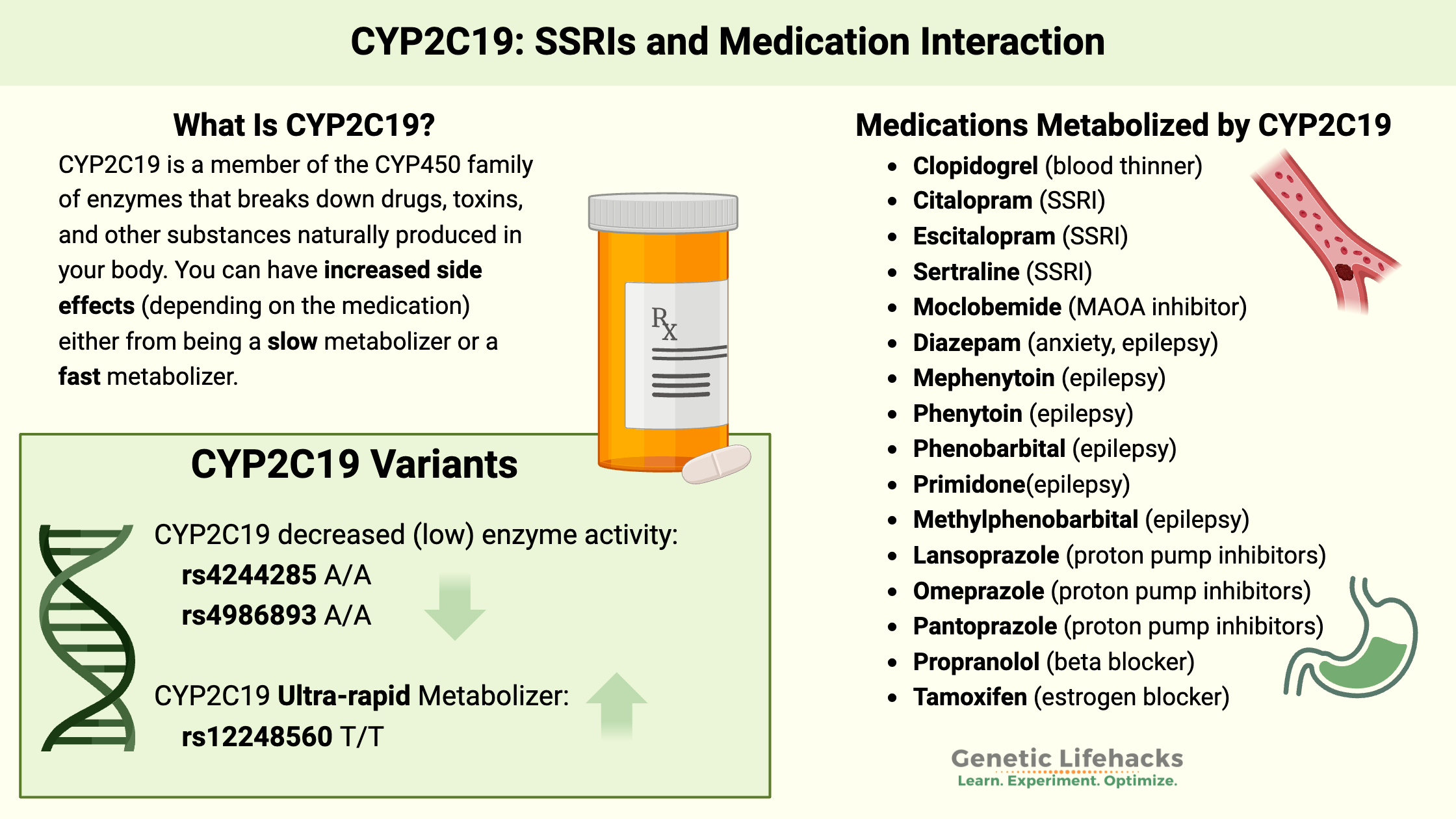
CYP2C19 is a member of the CYP450 family of enzymes that breaks down drugs, toxins, and other substances naturally produced in your body. (Learn more about other detoxification genes.)
The CYP2C19 enzyme is responsible for the breakdown (also called metabolism) of several popular drugs, including proton pump inhibitors (omeprazole, esomeprazole, lansoprazole), certain anti-epileptics, and an antiplatelet drug (clopidogrel).
Several important CYP2C19 genetic variants impact how drugs break down, causing some people to be poor metabolizers and others to be fast metabolizers.
You can have increased side effects (depending on the medication) either from being a slow metabolizer or a fast metabolizer.
Some medications, called pro-drugs, need to break down into their metabolites for the drug to be effective. Other drugs clear your system through the use of the CYP enzymes. Thus, the effect of a variant depends on the specific medication.
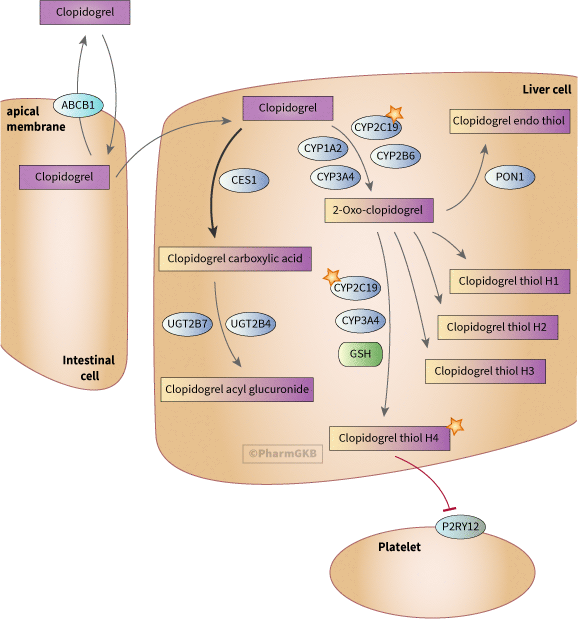
Here’s an example of the activation of the pro-drug clopidogrel (a blood thinner) by the CYP2C19 enzyme. Without a functioning CYP2C19 enzyme, the active thiol form of clopidogrel won’t be formed and thus blood clots will still be able to form.
CYP2C19 medication example:
Clinical trials clearly show that genetic variants (SNPs) in CYP2C19 can affect how people react to different medications.
- A CYP2C19 fast metabolizer taking omeprazole to treat h. pylori may have an insufficient response because the drug may not remain active in the body long enough.[ref]
- Alternatively, pro-drugs, such as clopidogrel, convert into their active drug state through CYP2C19. If you are a poor metabolizer, it could mean clopidogrel (an anticoagulant) isn’t activated enough, and you wouldn’t be protected from blood clots.[ref]
- Diazepam is another common drug metabolized partly by CYP2C19 (along with the CYP3A4 enzyme). Currently, there are no official recommendations to physicians as to reducing the dosages for poor metabolizers, but there is a box warning about CYP2C19.[ref]
- Some SSRIs, citalopram, sertraline, and escitalopram, also metabolize mainly through CYP2C19.[ref]
- A 2021 study showed that the average dose of citalopram is not as effective as an antidepressant for people with one copy of a non-functioning CYP2C19 variant (rs4244285).[ref]
CYP2C19 Poor Metabolizers:
You can your genetic data below to see if you are likely to be a poor metabolizer or have reduced CYP2C19 function. The frequency of poor metabolizers varies quite a bit by ancestry group:
- Approximately 10 – 20% of Asians are poor metabolizers, as are 2 – 5% of people of Caucasian descent.
- Up to 20-30% of Caucasians are fast metabolizers, but less than 5% of Asians are.
Medications metabolized by CYP2C19:
Many different medications are metabolized at least in part by CYP2C19.
The most important interaction is with clopidogrel (Plavix). People who have non-functioning CYP2C19 variants aren’t able to turn the pro-drug into the active form that acts as a blood thinner. This is a problem after heart surgery when someone depends on clopidogrel to block the formation of blood clots. CPIC Guidelines
Other commonly used drugs metabolized by CYP2C19 include:[ref]
- voriconazole (antifungal) – CPIC guidelines for CYP2c19
- citalopram (SSRI)
- escitalopram (SSRI)
- sertraline (SSRI)
- moclobemide (MAOA inhibitor)
- diazepam (anxiety, epilepsy)
- mephenytoin (epilepsy)
- phenytoin (epilepsy)
- phenobarbital (epilepsy)
- primidone(epilepsy)
- methylphenobarbital (epilepsy)
- lansoprazole (proton pump inhibitors)
- omeprazole (proton pump inhibitors)
- pantoprazole (proton pump inhibitors)
- propranolol (beta blocker)
- tamoxifen (estrogen blocker)
You can check for less common gene X drug interactions on DrugBank Online.
Natural supplements that interact with CYP2C19:
- limonene, found in citrus essential oil (inhibitor of CYP2c19)[ref]
- artemisinin (induces CYP2C19)
- quercetin (weak inhibitor)[ref]
- resveratrol (weak inhibitor)[ref]
Related article: Resveratrol: Genetic Interactions and Bioavailability
- berberine (weak inhibitor)[ref][ref]
Environmental toxins:
CYP2C19 is also involved in the metabolism of certain environmental toxins. When CYP enzymes break down toxins, the metabolite formed is often also toxic and needs to be quickly eliminated using phase II detoxification.
Diazinon is an organophosphate pesticide bioactivated by CYP2C19.[ref]
People with low CYP2C19 activity alongside higher CYP2B6 activity are more likely to have AChE activity inhibition with exposure to organophosphate pesticides (chlorpyrifos).[ref]
Endogenous substances metabolized by CYP2C19:
While we often focus on the interactions with drug metabolism, the CYP2C19 enzyme is found naturally in the body to break down several hormones that are endogenously produced.
- CYP2C19 helps to activate and break down some hormones, such as progesterone.[ref]
- It is involved (minor) in metabolizing melatonin[ref]
- It is also involved in the metabolism of estradiol.[ref]
Note that CYP2C19 is not the only route for metabolizing these hormones, just one way that the body can break them down.
CYP2C19 Genotype Report:
Access this content:
An active subscription is required to access this content.
Lifehacks:
Lifestyle interactions:
Stop smoking:
If you are a CYP2C19 poor metabolizer and a smoker, you have a 5x increased risk of lung cancer[ref] and a 17x increased risk of laryngeal cancer.[ref] Other studies show that CYP2C19 poor metabolizers are more likely to have esophageal cancer with smoking or pickled vegetable consumption.[ref]
Pharmacogenetic testing for antidepressants:
Access this content:
An active subscription is required to access this content.
Related Articles and Topics:
References:
Debbie Moon is a biologist, engineer, author, and the founder of Genetic Lifehacks where she has helped thousands of members understand how to apply genetics to their diet, lifestyle, and health decisions. With more than 10 years of experience translating complex genetic research into practical health strategies, Debbie holds a BS in engineering from Colorado School of Mines and an MSc in biological sciences from Clemson University. She combines an engineering mindset with a biological systems approach to explain how genetic differences impact your optimal health.