Key Takeaways:
~ The CYP450 family of enzymes breaks down (metabolizes) toxins, medications, and vitamin D.
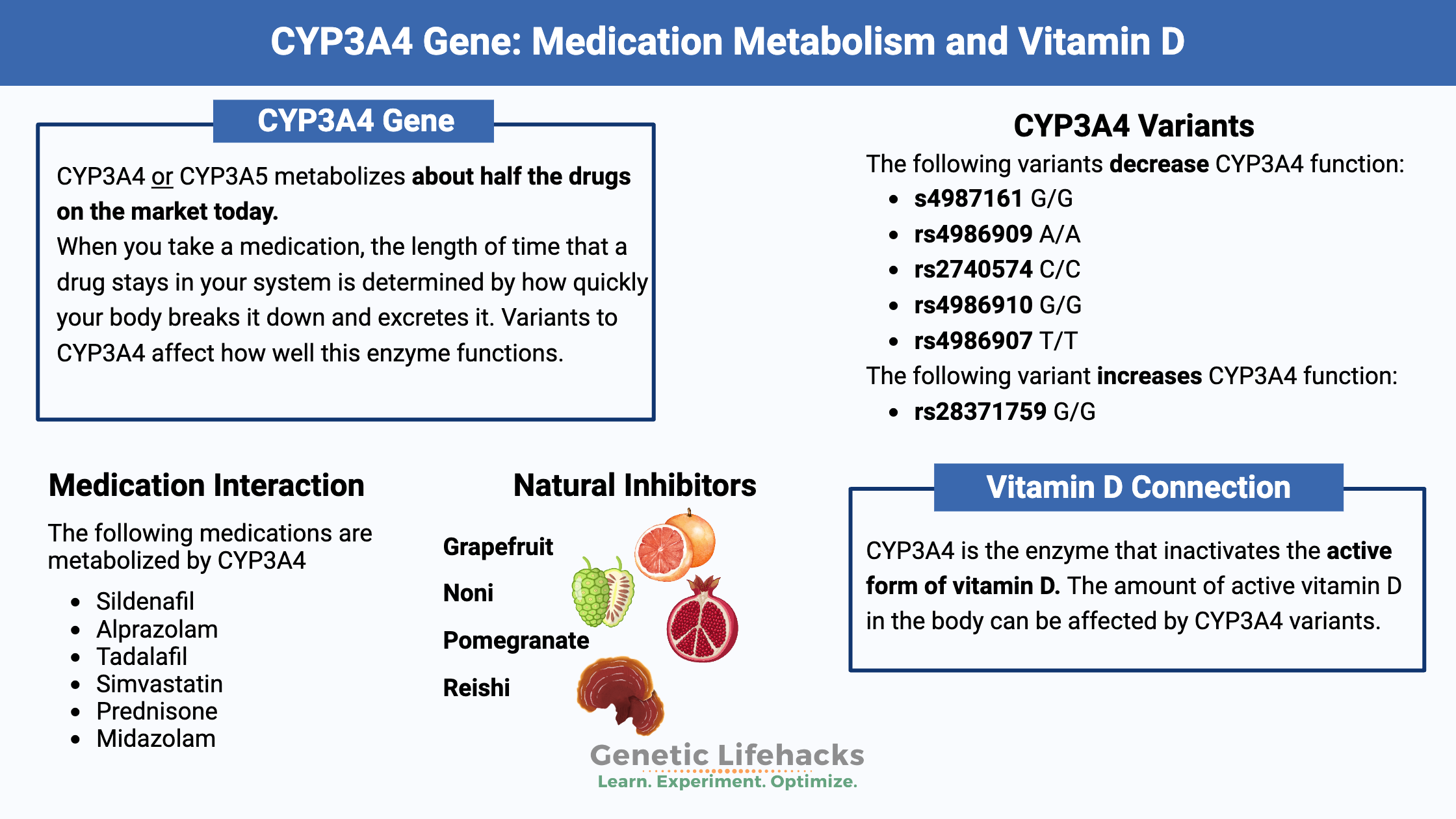
~ The CYP3A4 gene encodes the enzyme that metabolizes many commonly used drugs.
~ CYP3A4 genetic variants can impact whether someone clears a drug quickly or slowly, as well as how well a medication will work for an individual.
This article is part of a series of articles on phase I and phase II detoxification genes.
CYP3A4 and CYP3A5 enzymes and drug metabolism:
The CYP3A genes, which code for enzymes of the same name, are a subfamily of CYP450. The CYP450 enzymes are used by the body to break down and eliminate many different toxicants and medications.
CYP3A4 or CYP3A5 metabolizes about half the drugs on the market today, as well as other xenobiotics and steroids. When you take a medication, the length of time that a drug stays in your system is determined by how quickly your body breaks it down and excretes it.
There are genetic variants, or SNPs, in the CYP3A family that alter the function of the enzymes. These variants can impact how you react to a medication. For example, if you don’t break down a medication as quickly, you may need less of the medication over time. Similarly, if you metabolize a medication more quickly than normal, you may need to alter the timing or change the dosage.
Common medications cleared by CYP3A4:
Here are a few of the more commonly prescribed drugs that are metabolized and thus cleared from the body using the CYP3A4 enzyme:
- sildenafil
- alprazolam
- tadalafil
- simvastatin
- prednisone
- midazolam
Methadone dosages can also be impacted by this gene.[ref]
A full list of drugs metabolized by CYP3A4 is available on Pharmacy Times and Wikipedia.
Natural inhibitors of CYP3A4:
CYP3A4 can be impacted by commonly taken supplements and fruit juice.
CYP3A4 and Grapefruit:
Several fruits – grapefruit, noni, pomegranate – are potent inhibitors of CYP3A4. This means that the fruit blocks (inhibits) the enzyme from working. Eating or drinking grapefruit, noni, or pomegranates can cause adverse effects on drug metabolism, either increasing the efficiency of the drug or decreasing its effect.
Commonly used as medicinal mushrooms, Reishi (Lingzhi) may inhibit CYP3A4 and may change medication clearance rates. The study was done in animals, but it is something to be aware of if you are taking reishi along with medications (especially if you are washing it all down with grapefruit juice).[ref]
Inflammatory cytokines—interleukin (IL)-1β, IL-1α, IL-6, and TNF – can downregulate CYP3A4.[ref]
Resveratrol at 1,000 mg/day has been shown to inhibit CYP3A4, CYP2D6, and CYP2C9. It also induces CYP1A2.[ref] This is important because taking higher doses of resveratrol could interact with most prescription medications. Be sure to talk to your doctor or pharmacist before taking resveratrol in conjunction with other medications.
Related article: Resveratrol Studies, Genetic Interactions, and Bioavailability
Inducers of CYP3A4:
Dexamethasone and growth hormone induce CYP3A4 enzyme production. Phenobarbitol and high levels of bile acids can also induce CYP3A4 expression.[ref][ref]
Endogenous substances bioactivated by CYP3A4:
We don’t just have the CYP450 enzymes in the body to break down modern medications.
Vitamin D:
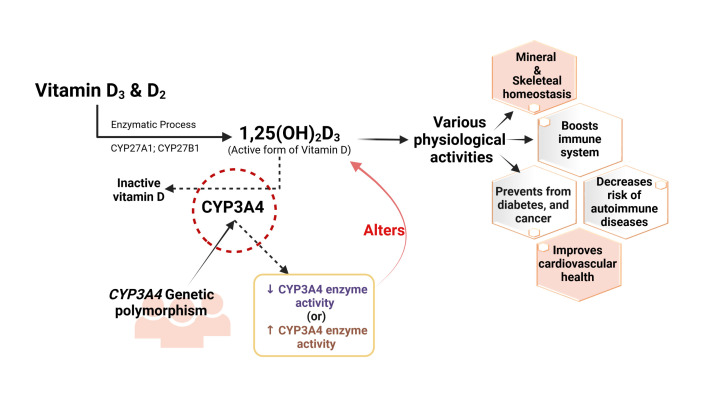
CYP3A4 is the enzyme that inactivates the active form of vitamin D (1,25(OH)2 D3). Thus, the amount of active vitamin D in the body can be affected by CYP3A4 variants that decrease the function of the enzyme. Some of the genetic variants that decrease CYP3A4 activity have been shown to increase 1,25(OH)2 D3 levels. Active vitamin D levels control calcium and bone density. CYP3A4 variants with increased enzyme activity are linked to an increased risk for low bone mineral density (BMD). [ref][ref]
Related article: Vitamin D – Genetic variants, receptor function
Testosterone:
CYP3A4 converts testosterone into three different hydroxylated metabolites: 6β-hydroxytestosterone (6β-OH-T), 2β-hydroxytestosterone (2β-OH-T), and 2α-hydroxytestosterone (2α-OH-T).[ref][ref]
Interestingly, the CYP3A4 enzyme is naturally more active in women than in men. This may cause differences in the way that women react to certain medications at higher doses.
Bile acids:
Bile acid metabolism and cholesterol metabolism can also involve CYP3A4.[ref]
Genotype Report: CYP3A4 and CYP3A5
Access this content:
An active subscription is required to access this content.
Lifehacks:
If you carry one or two copies of a CYP3A4 variant that is non-functioning, this may impact the way medications work for you. Look through the full list of drugs metabolized by this enzyme and talk with your doctor or pharmacist. (Keep in mind that 23andMe and AncestryDNA do not guarantee accuracy for medical purposes. Your doctor may want to run a second test to confirm.)
Grapefruit, noni, and pomegranate juices are inhibitors of CYP3A4 and CYP3A5. If you carry any of the genetic variants above for CYP3A4, be very careful of these juices or other inhibitors when taking a medication that is metabolized through CYP3A4.
St. John’s Wort is an inducer of CYP3A4, meaning it causes more of the enzyme to be created in the body. If you are taking a drug that is metabolized by CYP3A4, then you need to be careful with St. John’s wort interacting with the medication. (Talk with a doctor or pharmacist)[ref]
Access this content:
An active subscription is required to access this content.
Related Articles and Topics:
Lithium Orotate and Vitamin B12: Benefits for Mood and Cognitive Support
References:
John R. Horn, PharmD, and PharmD Philip D. Hansten. “Get to Know an Enzyme: CYP3A4.” Pharmacy Times, vol. 0, Sept. 2008. www.pharmacytimes.com, https://www.pharmacytimes.com/view/2008-09-8687.
Klein, Kathrin, and Ulrich M. Zanger. “Pharmacogenomics of Cytochrome P450 3A4: Recent Progress Toward the ‘Missing Heritability’ Problem.” Frontiers in Genetics, vol. 4, Feb. 2013, p. 12. PubMed Central, https://doi.org/10.3389/fgene.2013.00012.
Lamba, Jatinder, et al. “ClinPGx Summary: Very Important Pharmacogene Information for CYP3A5.” Pharmacogenetics and Genomics, vol. 22, no. 7, July 2012, pp. 555–58. PubMed Central, https://doi.org/10.1097/FPC.0b013e328351d47f.
Lee, Su-Jun, and Joyce A. Goldstein. “Functionally Defective or Altered CYP3A4 and CYP3A5 Single Nucleotide Polymorphisms and Their Detection with Genotyping Tests.” Pharmacogenomics, vol. 6, no. 4, June 2005, pp. 357–71. PubMed, https://doi.org/10.1517/14622416.6.4.357.
Richards-Waugh, Lauren L., et al. “Fatal Methadone Toxicity: Potential Role of CYP3A4 Genetic Polymorphism.” Journal of Analytical Toxicology, vol. 38, no. 8, Oct. 2014, pp. 541–47. PubMed, https://doi.org/10.1093/jat/bku091.
Sprouse, Alyssa A., and Richard B. van Breemen. “Pharmacokinetic Interactions between Drugs and Botanical Dietary Supplements.” Drug Metabolism and Disposition, vol. 44, no. 2, Feb. 2016, pp. 162–71. PubMed Central, https://doi.org/10.1124/dmd.115.066902.