Key takeaways:
~ Factor V is an important protein in the clotting process, and mutations in the F5 gene can lead to conditions like hemophilia, characterized by poor clotting ability.
~The factor V Leiden variant causes an increased risk of clotting by resisting the shutoff signal from activated protein C. This leads too larger clots that can obstruct blood flow.
~ People with the factor V Leiden variant are at a higher risk of developing deep vein thrombosis (DVT) and pulmonary embolism, with a four-fold increase for one copy and an eleven-fold increase for two copies of the variant.
When you get a cut or wound, a cascade of events takes place in the body.
Blood Clotting and Factor V Leiden:
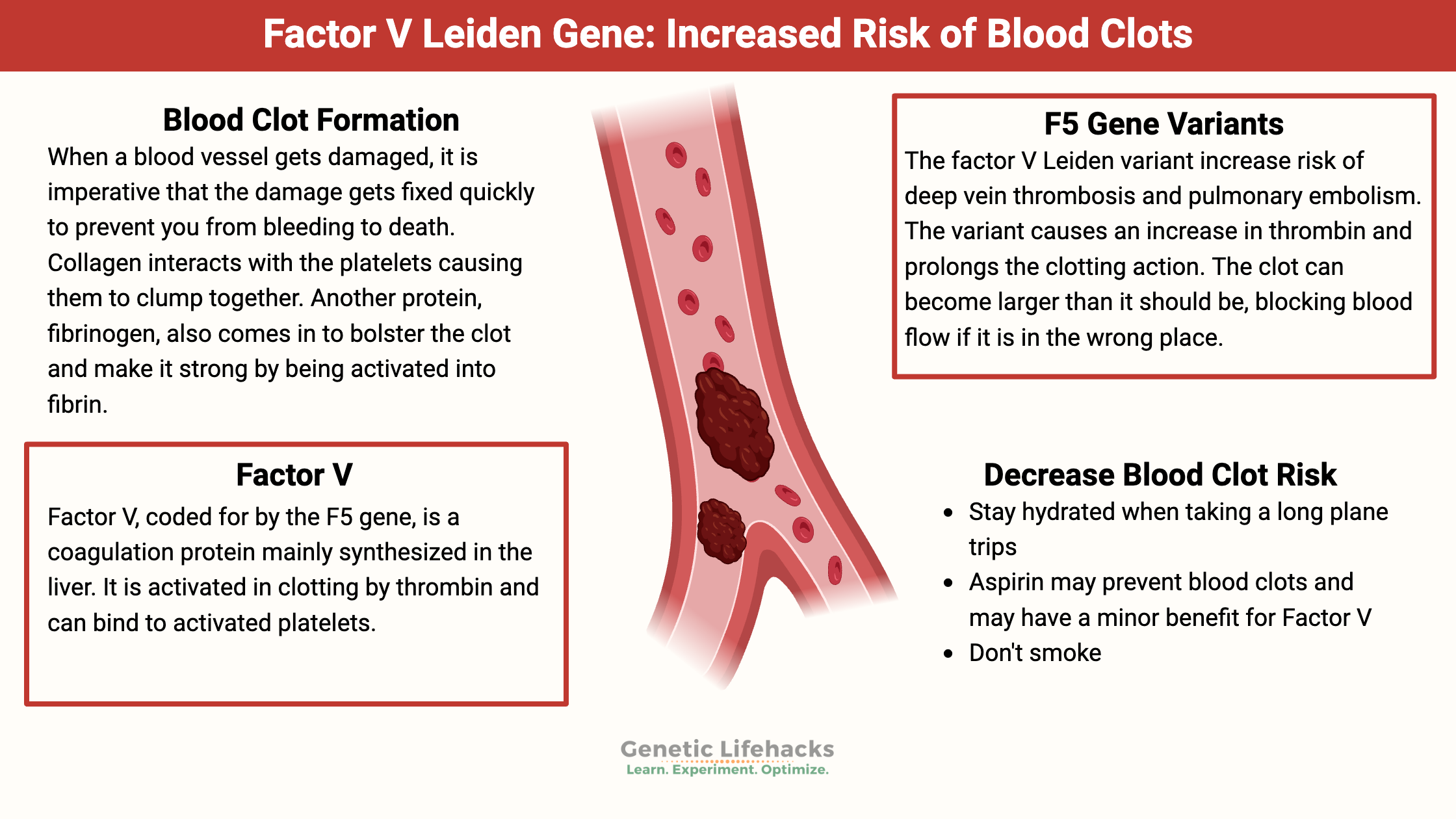
Blood vessels are made of endothelial cells, which are tightly joined together. When a blood vessel gets damaged, it is imperative that the damage gets fixed quickly to prevent you from bleeding to death.
The platelets in your blood clump together to form a clot blocking the damaged part of the blood vessel. Platelets flow through your blood vessels all the time without clumping together, so the body activates the clotting when needed.
Collagen, which is located on the outside of the blood vessels, interacts with the platelets causing them to clump together. Another protein, fibrinogen, also comes in to bolster the clot and make it strong by being activated into fibrin. A cascade of events takes place here quickly to activate the fibrinogen. Thrombin is the main activator and turns fibrinogen into fibrin.
Within this cascade, many ‘factors’ are present and integral to the process, and they are referred to as ‘factor’ plus a Roman numeral (e.g., factor V and factor VIII).
Factor V, coded for by the F5 gene, is a coagulation protein mainly synthesized in the liver. It is activated in clotting by thrombin and can bind to activated platelets. Just as there is a cascade of events that quickly causes a blood clot to form, other molecules are involved, such as protein C, in turning off the clotting when it is no longer needed.[ref]
Mutations that cause a deficiency in factor V cause mild forms of hemophilia or an inability to clot well. More severe forms of hemophilia are caused by a mutation in other factor genes (e.g., factor IX mutation caused the type of hemophilia in European royal families).
Factor V Leiden variant:
Conversely, the factor V Leiden variant causes the opposite problem from hemophilia. A change in the gene causes a more active version to resist the shutoff signal from activated protein C and stay active, thus increasing thrombin and prolonging the clotting action. The clot can become larger than it should be, blocking blood flow if it is in the wrong place.
Factor V Leiden has been linked in many studies to an increased risk of deep vein thrombosis and pulmonary embolism. A meta-analysis that combined data from 31 studies estimates that the increase in the risk of thrombosis for people carrying one copy of the variant was 4-fold, and the increase for those carrying two copies was 11-fold.[ref][ref][ref][ref]
This does not mean that everyone who carries the factor V Leiden will have a deep vein thrombosis (DVT) or pulmonary embolism — but they are at a statistically higher risk. The CDC estimates the per year incidence of DVT is 1 to 2/1000 people.[ref] An 11-fold increase in risk for someone who is homozygous for the variant would then indicate a 1 to 2% risk of DVT in a given year.
Factor V Leiden has also been linked in studies to an increased risk of miscarriage.[ref][ref] The risk may be higher for women who are homozygous for the variant. One study found that the rate of live births for non-carriers of factor V Leiden was 85%. Women who carried one copy of the variant had an 84% live birth rate, and women who carried two copies of the variant had an 80% live birth rate.[ref]
A good source of information on thrombosis and clotting disorders is Clot Connect, from the University of North Carolina.
The factor V Leiden variant is found in about 5-8% of people of European descent. Researchers have several theories of why such a deleterious mutation has been passed down at a higher rate. Interestingly enough, one advantage of clotting more readily would be for women in childbirth, which historically included high rates of hemorrhaging. In times of war, it would also be an advantage to clot a little better when wounded. And finally, there is a statistically higher sperm count found in men who are carriers of the factor V Leiden variant, so the mutation would have been slightly more likely to be passed on to more offspring.[ref][ref][ref]
Factor V Leiden Genotype Report
🖨 Printable Overview (Members)
Check your genetic data for rs6025 (23andMe v4, v5; AncestryDNA):
- C/C: typical
- C/T: one copy of factor V Leiden
- T/T: two copies of factor V Leiden
Members: Your genotype for rs6025 is —.
[/mepr-show]
Lifehacks:
Talk to Your Doctor:
Your doctor should know, based on all of your medical history, whether you should take preventative medications for thrombosis. Also, keep in mind that 23andMe data is not guaranteed to be 100% accurate, so a clinical test should be done to verify the results before taking medical action.
The question that may come to mind here is whether talking with your doctor about carrying the genetic variant for factor V Leiden will raise your insurance rates. In the US, your health insurance company cannot raise your rates due to the results of a genetic test. That is not true, though, for life insurance companies and long-term care insurance, who may (or may not) make their rates dependent on genetic information in your electronic health records.
Suggestions to decrease blood clot risk:
Access this content:
An active subscription is required to access this content.
Related Articles and Topics:
Plasminogen Activator Inhibitor-1 (PAI-1): Regulator of Clotting
References:
Arsov, Todor, et al. “Factor V Leiden Is Associated with Higher Risk of Deep Venous Thrombosis of Large Blood Vessels.” Croatian Medical Journal, vol. 47, no. 3, June 2006, pp. 433–39. PubMed Central, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2080416/.
Biron-Andréani, Christine, et al. “Factor v Leiden Homozygous Genotype and Pregnancy Outcomes.” Obstetrics and Gynecology, vol. 114, no. 6, Dec. 2009, pp. 1249–53. PubMed, https://doi.org/10.1097/AOG.0b013e3181c2243d.
Campello, Elena, et al. “Diagnosis and Management of Factor V Leiden.” Expert Review of Hematology, vol. 9, no. 12, Dec. 2016, pp. 1139–49. PubMed, https://doi.org/10.1080/17474086.2016.1249364.
CDC. “Data and Statistics on Venous Thromboembolism | CDC.” Centers for Disease Control and Prevention, 25 Apr. 2022, https://www.cdc.gov/ncbddd/dvt/data.html.
Cohn, D. M., et al. “Increased Sperm Count May Account for High Population Frequency of Factor V Leiden.” Journal of Thrombosis and Haemostasis: JTH, vol. 8, no. 3, Mar. 2010, pp. 513–16. PubMed, https://doi.org/10.1111/j.1538-7836.2009.03710.x.
El-Galaly, T. C., et al. “Interaction between Blood Type, Smoking and Factor V Leiden Mutation and Risk of Venous Thromboembolism: A Danish Case-Cohort Study: Letters to the Editor.” Journal of Thrombosis and Haemostasis, vol. 10, no. 10, Oct. 2012, pp. 2191–93. DOI.org (Crossref), https://doi.org/10.1111/j.1538-7836.2012.04772.x.
Glynn, Robert J., et al. “Effect of Low-Dose Aspirin on the Occurrence of Venous Thromboembolism: A Randomized Trial.” Annals of Internal Medicine, vol. 147, no. 8, Oct. 2007, pp. 525–33. PubMed, https://doi.org/10.7326/0003-4819-147-8-200710160-00004.
Hovens, M. M. C., et al. “Aspirin in the Prevention and Treatment of Venous Thromboembolism.” Journal of Thrombosis and Haemostasis: JTH, vol. 4, no. 7, July 2006, pp. 1470–75. PubMed, https://doi.org/10.1111/j.1538-7836.2006.01928.x.
Jusić, Amela, et al. “The Association of Factor V G1961A (Factor V Leiden), Prothrombin G20210A, MTHFR C677T and PAI-1 4G/5G Polymorphisms with Recurrent Pregnancy Loss in Bosnian Women.” Medicinski Glasnik: Official Publication of the Medical Association of Zenica-Doboj Canton, Bosnia and Herzegovina, vol. 15, no. 2, Aug. 2018, pp. 158–63. PubMed, https://doi.org/10.17392/948-18.
Juul, Klaus, et al. “Factor V Leiden and the Risk for Venous Thromboembolism in the Adult Danish Population.” Annals of Internal Medicine, vol. 140, no. 5, Mar. 2004, pp. 330–37. PubMed, https://doi.org/10.7326/0003-4819-140-5-200403020-00008.
(No Title). https://clotconnect.wpcomstaging.com/. Accessed 18 Oct. 2022.
Ridker, P. M., et al. “Factor V Leiden Mutation as a Risk Factor for Recurrent Pregnancy Loss.” Annals of Internal Medicine, vol. 128, no. 12 Pt 1, June 1998, pp. 1000–03. PubMed, https://doi.org/10.7326/0003-4819-128-12_part_1-199806150-00007.
Saeed, Anjum, et al. “To Determine the Frequency of Factor V Leiden in Cases of Deep Vein Thrombosis and Healthy Controls.” Pakistan Journal of Medical Sciences, vol. 31, no. 5, Oct. 2015, pp. 1219–22. PubMed, https://doi.org/10.12669/pjms.315.8088.
Simone, Benedetto, et al. “Risk of Venous Thromboembolism Associated with Single and Combined Effects of Factor V Leiden, Prothrombin 20210A and Methylenetethraydrofolate Reductase C677T: A Meta-Analysis Involving over 11,000 Cases and 21,000 Controls.” European Journal of Epidemiology, vol. 28, no. 8, Aug. 2013, pp. 621–47. PubMed, https://doi.org/10.1007/s10654-013-9825-8.
Thrombophilia and Insurance. 10 Aug. 2011, https://clotconnect.wpcomstaging.com/2011/08/10/thrombophilia-and-insurance/.
van Mens, T. E., et al. “Factor V Leiden Is Associated with Increased Sperm Count.” Human Reproduction (Oxford, England), vol. 32, no. 11, Nov. 2017, pp. 2332–39. PubMed, https://doi.org/10.1093/humrep/dex287.
van Mens, Thijs E., et al. “Evolution of Factor V Leiden.” Thrombosis and Haemostasis, vol. 110, no. 1, July 2013, pp. 23–30. PubMed, https://doi.org/10.1160/TH13-02-0115.