Key takeaways:
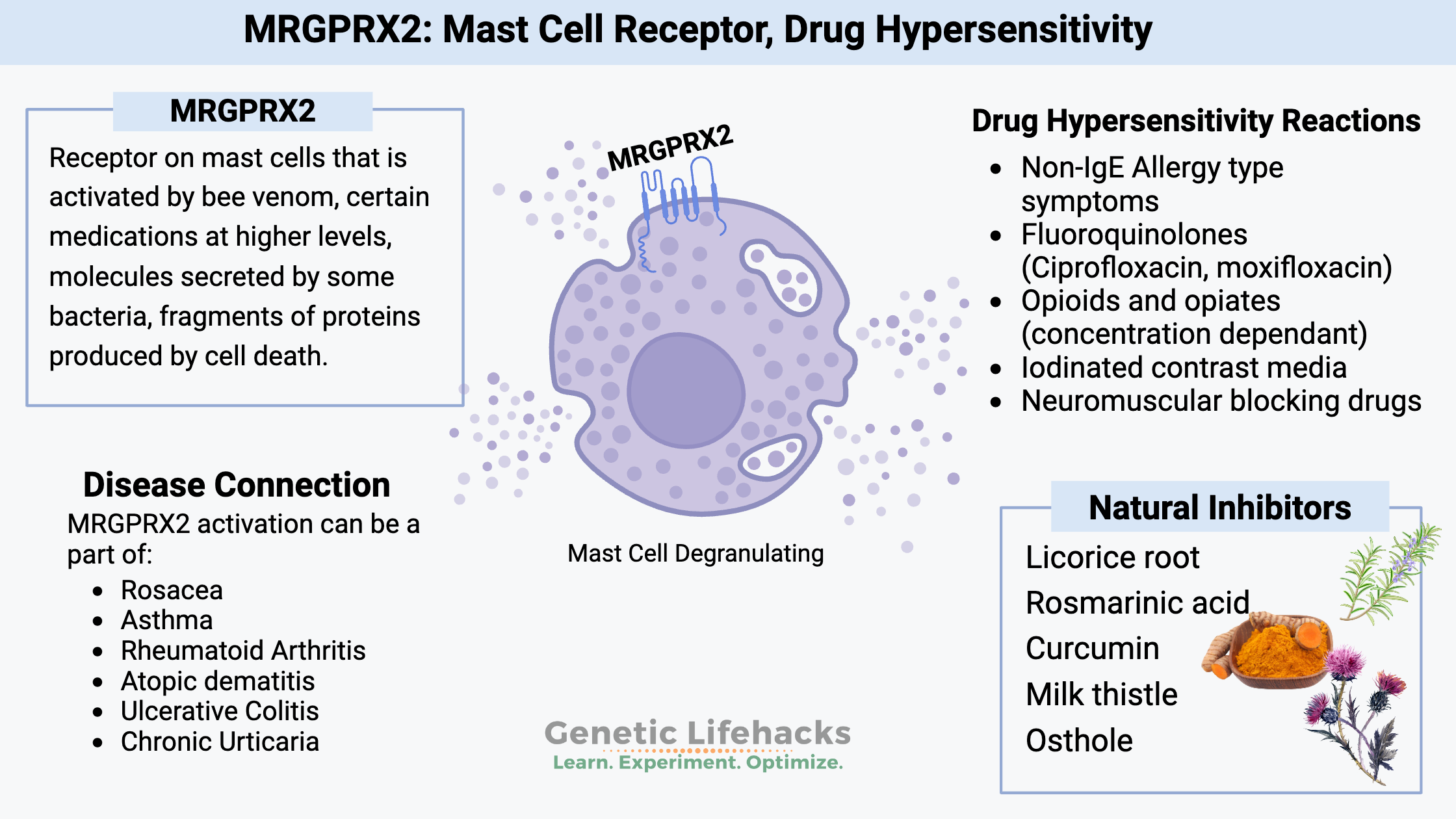
~ Hypersensitivity reactions to drugs, especially fluoroquinolones or contrast media, can be due to mast cell activation by the MRGPRX2 receptor.
~ The MRGPRX2 receptor is found on mast cells and certain types of neurons. It can be activated by protein fragments, certain types of drugs, bee venom, and antimicrobial host defense peptides.
~ Genetic research on this receptor is still relatively new, but there are a couple of known SNPs that affect MRGPRX2 function.
Members will see their genotype report below and the solutions in the Lifehacks section. Consider joining today.
MRGPRX2 activation can cause reactions that are not “true allergies”:
Some people seem to be allergic to everything, from medications and supplements to seemingly everything inside them. Yet traditional allergy tests show that they aren’t allergic to anything. Researchers call these types of reactions ‘hypersensitivity’ or ‘pseudoallergic’ reactions.[ref]
At the heart of some hypersensitivity reactions is the MRGPRX2 receptor. This receptor has also been linked to itching and skin conditions, such as rosacea and atopic dermatitis, as well as ulcerative colitis.[ref]
What is MRGPRX2?
MRGPRX2, or Mas-related G protein-coupled receptor X2, is a member of a family of proteins that play key roles in sensory perception and inflammation.
It is primarily expressed on the surface of mast cells, which are immune cells involved in allergic reactions, inflammation, and defense against bacteria and viruses.
There are multiple triggers that activate mast cells. Allergic reactions are traditionally caused by IgE allergen activation, where exposure to an allergen triggers the immune response. However, there are other ways that mast cells can be triggered that are different from traditional IgE allergen activation.
For a long time, the allergy-type reactions that didn’t involve IgE and traditional allergy pathways were lumped together under the term “non-IgE”. It turns out that there are more ways to activate mast cells than originally thought.
Mast cells can also be activated by binding to certain pathogens or toxins, or even by substances like histamine causing additional mast cell degranulation.
MRGPRX2 is unique in that it is involved in non-IgE mast cell activation – not the typical allergy reaction. MRGPRX2 has a wide range of activators and is thought to play a role in inflammatory skin conditions, asthma, and pain.
Most of the research on MRGPRX2 is fairly recent. And researchers are realizing that this gene may be important in understanding the mystery of pseudo-allergic type reactions.
Background on Mast Cells:
The MRGPRX2 receptor is found on mast cells, as well as a few other types of cells, which we will get to in a minute. First, let’s take a look at mast cells.
Mast cells are a type of immune cell found throughout the body. They are most abundant in areas exposed to pathogens, such as the skin, lungs, and intestines. They can also be found in connective tissue.
As a first line of defense, mast cells can react strongly to fight off anything perceived as a foreign invader. They aren’t specific to a particular virus or bacteria, but respond to many different classes of molecules. The only metaphor that comes to mind is war: mast cells are like land mines that go off when triggered by something, while other immune responses are like strategic drone strikes on a specific target. (Interesting tidbit: Mast cells are found in all animals and are thought to be an ancient form of pathogen defense, found in 500-million-year-old invertebrates[ref])
There are two types of mast cells:[ref]
- Tryptase-expressing mast cells are found in the lungs and intestines.
- Chymase and tryptase-expressing mast cells are found primarily in connective tissues such as the skin and myocardium (heart muscle). MRGPRX2 is primarily found in these connective tissue mast cells.
Activation of mast cells causes the release of several different compounds that cause changes, such as vasodilation or nerve activation.
Mast cells are primed and ready to respond to allergens, foreign particles, and pathogens with mediators that are stored in granules, ready to be released in an instance.
- Mast cells release histamine, which causes itching (urticaria), vasodilation, and other reactions, depending on where the mast cells are activated.
- Mast cells can also release tryptase, which causes flushing, airway reactions, and gastrointestinal changes.[ref]
- Inflammatory cytokines, heparin, and lipid mediators can also be released, depending on where in the body the mast cells are located and how they are activated.
What activates the MRGPRX2 receptor?
MRGPRX2 receptors have only recently been identified, so researchers are still figuring out everything that activates them. MRGPRX2 is classified as a G protein-coupled receptor (GPCR), which is a type of receptor that passes through a cell membrane and is activated by an agonist.
A ligand is a natural molecule in the body that binds to a receptor and acts as an agonist to stimulate the response. MRGPRX2 appears to have a number of different ligands that can bind to it and activate it.
MRGPRX2 ligands that activate the receptor include: [ref][ref][ref]
- Antimicrobial host defense peptides, such as LL-37
- Quorum-sensing molecules secreted by bacteria
- Fragments of proteins, such as albumin fragments or fragments due to cell death
- Neuropeptides such as substance P
- Peptide found in bee or wasp venom
- And… certain types of medications at the right levels
Let’s look at the medication-related hypersensitivity reactions first, and then go into the other ligands.
Drug reactions and MRGPRX2 receptor activation:
Some people experience allergy-like reactions, including anaphylaxis, when they take certain medications. Research now shows that this is often due to the activation of mast cells via MRGPRX2 receptors, rather than traditional allergic reaction pathways.[ref] This is why hypersensitivity reactions can be so frustrating because traditional allergy tests won’t show the reaction.
Allergic or anaphylactic reactions due to activation of MRGPRX2 on mast cells are found in several drug groups, including certain opioids, fluoroquinolone antibiotics, iodinated contrast media (e.g. in a CT scan), neuromuscular blocking agents, and a few antidepressants. [ref]
| Drug Class | Example Drugs | Possible Reactions | Notes |
|---|---|---|---|
| Fluoroquinolones | Ciprofloxacin, etc. | Itching, hives, anaphylaxis | More likely at higher concentrations |
| Opiates/opioids | Morphine, etc. | Granulomas, skin reactions | Concentration-dependent |
| Neuromuscular blocking drugs | Rocuronium | Anaphylaxis | Rare |
| Iodinated contrast media | — | Hives, swelling, severe rxns | 3% react; rate of delivery matters |
Fluoroquinolone reactions:
Antibiotics such as ciprofloxacin and moxifloxacin are classified as fluoroquinolone antibiotics (often called quinolones). Ciprofloxacin and topical fluoroquinolones used in eye drops can cause hypersensitivity reactions by activating mast cells via MRGPRX2. Higher concentrations of fluoroquinolones are more likely to trigger mast cell degranulation.[ref]
Opioids and opiates:
Opiates can activate mast cells via the MRGPRX2 receptors. Researchers show that this is a concentration-dependent activation that occurs more often in skin mast cells, which contain a high number of MRGPRX2 receptors.[ref] Other research shows that the MRGPRX2 receptor on mast cells is involved in granuloma formation from morphine infusion.[ref]
Neuromuscular blocking drugs:
Rocuronium is a neuromuscular blocking agent used in general anesthesia. Although rare, anaphylactic reactions can occur, and researchers have recently discovered that these reactions are driven by MRGPRX2 activation.[ref]
Iodinated contrast media:
About 3% of people have a reaction to iodinated contrast media, which is often used in CT scans and angiography. Most of the time, the reaction is mild, such as hives or swelling, but in a small percentage of cases, the reaction can be severe or even fatal. [ref] The contrast agent activates mast cells via the MRGPRX2 receptor. Similar to the above drugs, the mast cell degranulation appears to be concentration-dependent, with higher concentrations activating mast cells.[ref]
Tipping point: what pushes you over the edge and into mast cell activation?
A common thread in the research on mast cell activation by drugs is that the concentration needs to be at a certain level.
Drugs given intravenously enter the system faster, and the rate at which the drug is given plays a role in triggering hypersensitivity reactions.
A combination of drugs that activate MRGPRX2 could also elicit a hypersensitivity response. Genetic variants related to drug metabolism may also play a role.
Another component is whether the mast cells have upregulated MRGPRX2 expression or whether someone has an increased number of mast cells (e.g. mastocytosis).[ref]
For example, a study showed that drug sensitivity reactions were more likely to occur in people with a previous diagnosis of chronic urticaria, asthma, or mast cell activation disorder.[ref]
Endogenous ligands:
Ligands are the various natural compounds produced in the body that activate a receptor.
The first endogenous ligand for MRGPRX2 was found to be fragments of albumin. Albumins are proteins found in blood plasma that can bind to various substances to transport them throughout the body. Essentially, it is a water-soluble protein that makes up about 50% of plasma and regulates blood volume through an osmotic effect.[ref]
Interestingly, albumin fragments can be produced by mast cell degranulation, so this gives a possible mechanism for continued, self-perpetuating mast cell activation.[ref]
Endogenous protein and enzyme fragments have also been found to activate the MRGPRX2 receptor. Researchers think that MRGPRX2 reacts to “protein breakdown products released from damaged or dying cells.”[ref]
Neurokinins can also activate MRGPRX2.
Substance P is one neurokinin, found in the brain, sensory neurons, and the gastrointestinal tract. It is normally a pain signal that activates a neurokinin receptor, but it was recently discovered that substance P can bind to the MRGPRX2 receptor and induce mast cell degranulation.[ref]
IgG from people with fibromyalgia has been shown to activate mast cells through the MRGPRX2 receptor(preprint). [ref]
Diseases that involve MRGPRX2 activation:
MRGPRX2 has been implicated in several chronic diseases, including:
- Rosacea[ref]
- Asthma[ref]
- Atopic dermatitis[ref]
- Rheumatoid arthritis[ref]
- Ulcerative colitis[ref][ref]
- Chronic urticaria (itchiness, hives)[ref]
- Fibromyalgia (maybe)[ref]
While for some of these conditions, such as rosacea, the mast cell activation component has been known, it is a fairly recent discovery that the MRGPRX2 receptor binding is what causes the mast cell activation.[ref] Hopefully, this will lead to ways to block this activation to prevent inflammation and itching.
Mastocytosis: Systemic mastocytosis is a disease that causes an excess of mast cells to be produced in different organs of the body. In the skin, systemic mastocytosis can cause a reddish-brown lesion, called maculopapular cutaneous mastocytosis. The mast cells involved in the skin symptoms of mastocytosis have recently been found to have increased MRGPRX2 expression.[ref]
Lactic acid inhibits MRGPRX2:
For cell receptors, there are usually ligands that bind to them and turn them on, and then, on the other side of the equation, inhibitors that can block their activation.
One inhibitor of MRGPRX2 activation is lactic acid.[ref]
While we often think of lactic acid in terms of sore muscles after a hard workout, there are other causes of elevated lactic acid, such as asthma, cancer, thiamine deficiency, and certain infections. It is interesting that lactic acid acts to tamp down the overactivation of mast cells.
Desensitization of the receptor:
G protein-coupled receptors (GPCR) can become desensitized after repeated or prolonged exposure. One way receptors can be desensitized is through phosphorylation and then being bound to an arrestin.
Beta-arrestin-2 has been identified as the signal terminator for MRGPRX2, and beta-arrestin-1 is involved in controlling the abundance of the receptor.[ref] You’ll see in the genotype report below that one of the variants of MRGPRX2 is more easily desensitized by beta-arrestin, resulting in less mast cell degranulation.
Beyond mast cells: MGRPRX2 on neurons, basophils, and eosinophils
MRGPRX2 is also found as a receptor on some types of neurons.
The dorsal root ganglion is a collection of sensory neurons that carry messages from the periphery to the central nervous system. Essentially, they relay sensory information, like pain, heat, and touch, from your body to the spine and brain.
MGRPRX2 is found on the small-diameter sensory neurons of the dorsal root ganglion.[ref]
Basophils and eosinophils can also express the MGRPRX2 receptor. Basophils and eosinophils are types of white blood cells that can be involved in the immune response to allergens.
Some research shows that basophils have very low expression of the MRGPRX2 receptor under normal conditions, but when coupled with an IgE allergy, they can express more MRGPRX2 receptors. [ref][ref]
Genotype Report: MRGPRX2
Note: There are only a couple of variants of interest for MRGPRX2 in 23andMe or AncestryDNA data. This is likely due to the research on the gene being relatively recent. There are four other known rare mutations that also impact the function of the receptor that are not included in 23andMe or AncestryDNA data.
The variants identified have to do with reduced receptor function, meaning that some people are less likely to have degranulation of mast cells in response to medications, etc.
Check your genetic data for rs10833049 N62S (i6060783 23andMe v4, v5):
- T/T: typical mast cell activation
- T/C: somewhat decreased receptor function
- C/C: decreased receptor function, decreased mast cell activation[ref], receptor more easily dampened or desensitized, protective in ulcerative colitis.[ref]
Members: Your genotype for rs10833049 is — or for i6060783 is — .
Check your genetic data for rs11024970 N16H (23andMe v4; AncestryDNA):
- T/T: typical
- G/T: slight change to MRGPRX2 receptor, responds to pain stimulation (substance P) and slightly increased response to other stimuli [ref]
- G/G: change to MRGPRX2 receptor, responds to pain stimulation (substance P) and slightly increased response to other stimuli [ref]
Members: Your genotype for rs11024970 is —.
Lifehacks:
If you think that mast cell activation via the MRGPRX2 receptor is playing a role in any mast cell reactions you are having, keep an eye out for new research, and talk with your doctor to see if they know about any clinical trials.
Pharmaceutical companies are trying to develop drugs that act as antagonists for MRGPRX2. Escient Pharmaceuticals is one that has a small-molecule oral drug in development.[ref]
Contrast Media Precautions:
- If you’ve previously reacted to iodinated contrast media, notify your doctor before future procedures.
- Discuss the rate and method of administration, and consider sharing relevant MRGPRX2 research with your healthcare team..[ref]
Fluoroquinolone Reaction?
- If you have a history of reactions to fluoroquinolone antibiotics (MRGPRX2-related or otherwise), investigate ongoing clinical studies, such as those referenced at fq100.org.
5 Natural MRGPRX2 inhibitors:
Access this content:
An active subscription is required to access this content.
Related articles:
Histamine Intolerance: Genetic Report, Supplements, and Real Solutions
References: