You may have read or heard that anyone who carries MTHFR variants should not be vaccinated. Usually, the reason given is that those with decreased MTHFR enzyme activity cannot detoxify or ‘handle’ vaccinations, often with references to mercury in the vaccines.
This article reviews the published scientific studies on the topic of MTHFR and vaccinations. The intent is to inform and educate, based on research on the topic.
MTHFR and Vaccinations:
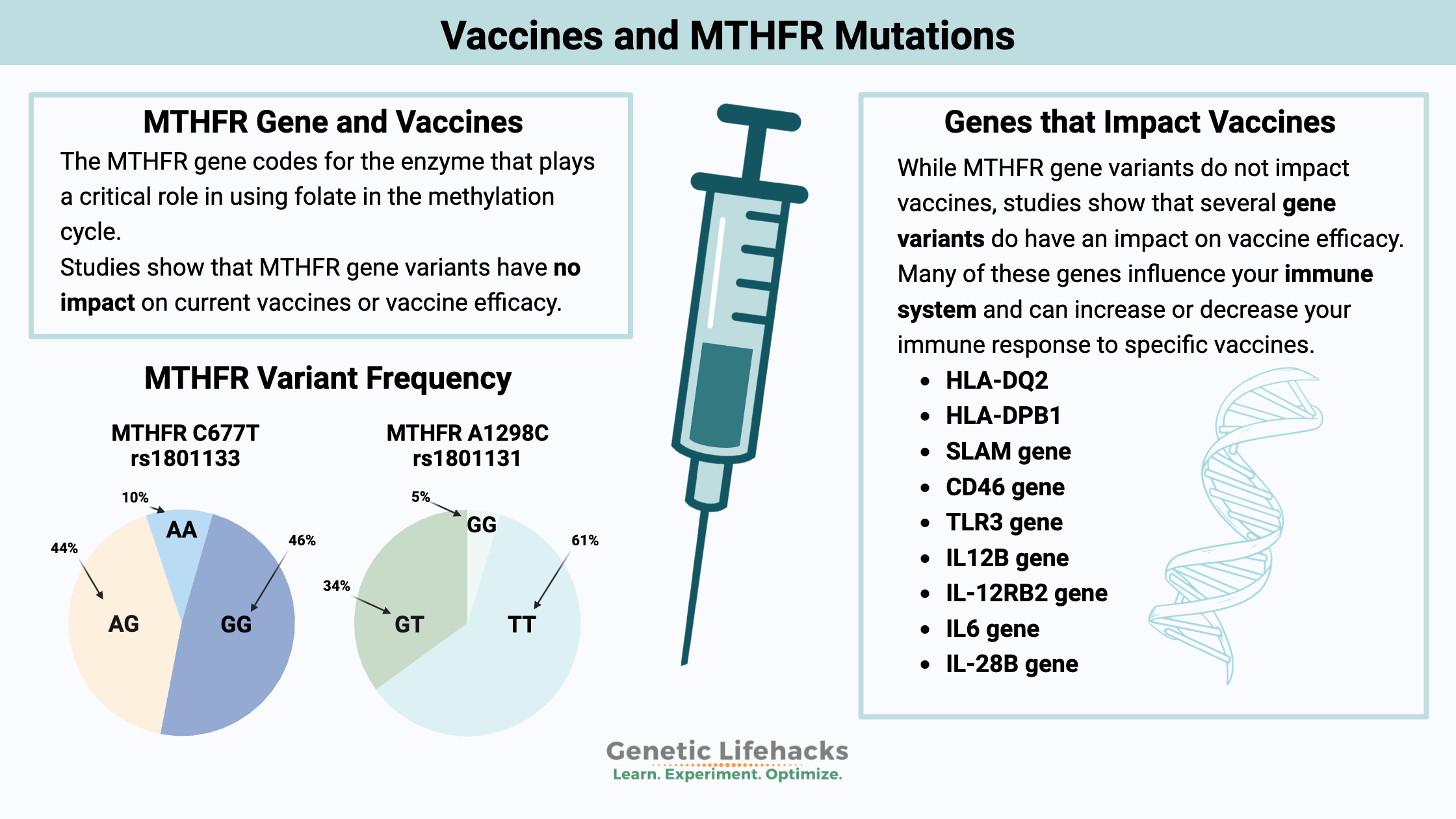
The MTHFR gene codes for the enzyme that plays a critical role in using folate in the methylation cycle.
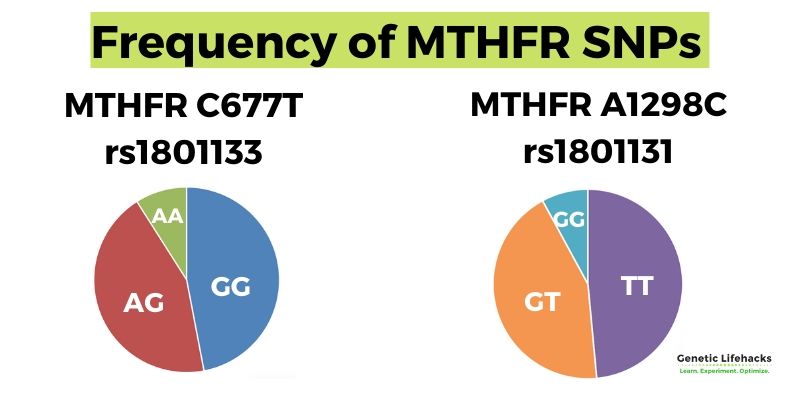
There are two genetic variants of MTHFR that many researchers have focused on. These two variants are known as C677T and A1298C.
If you have done 23andMe or AncestryDNA, you can check your raw data to see if you carry the variants.
MTHFR Genotype Report
Not a member? Join Here.
Membership lets you see your data right in each article and also gives you access to the members’ only information in the Lifehacks sections.
Check your genetic data for rs1801133 (23andMe v4, v5; AncestryDNA):
- G/G: typical *
- A/G: one copy of MTHFR C677T allele (heterozygous), function decreased by 40%
- A/A: two copies of MTHFR C677T (homozygous), function decreased by 70 – 80%
Members: Your genotype for rs1801133 is —.
Check your genetic data for rs1801131 (23andMe v4, v5; AncestryDNA):
- T/T: typical *
- G/T: one copy of MTHFR A1298C (heterozygous), slightly decreased enzyme function
- G/G: two copies of MTHFR A1298C (homozygous), decreases enzyme function by about 20%
Members: Your genotype for rs1801131 is —.
You can read all about the methylation cycle and the MTHFR gene here.
MTHFR Variants, not Mutations…
I purposefully refer to the genetic change in MTHFR as a variant instead of a mutation.
At least one copy of the C677T variant is found in more than half the people in most population groups. This is not a rare mutation, but rather a common variant that causes a change in how the gene functions.
Studies on MTHFR C677T and vaccines:
Researching the studies on MTHFR variants and vaccination injuries or adverse events lead me to exactly one study.
Seriously. One study — on a vaccine that is no longer given. It is an open-access article (freely accessible) on genetic variants and adverse reactions to the smallpox vaccine.
Overview of the study: In a study conducted by Vanderbilt University, 131 people (average age of 23) received a vaccine for smallpox. The results showed that those individuals with an MTHFR C677T variant were more likely to have an adverse reaction to the vaccination. The study also linked other genes to an increase in adverse events.
Adverse events were defined as a skin reaction at the site of injection, fever within 30 days of the vaccine, or enlarged or tender lymph nodes. Forty study participants reacted to the vaccine and 69 participants did not.[ref] Smallpox vaccines have not been used on the general public in the US in over 47 years, and none of the study participants had previously received a smallpox vaccine.[ref]
Read why the author of that smallpox vaccine study does NOT think it shows a reason not to vaccinate.
What about studies on MTHFR and vaccine excipients?
Some claim that excipients added to vaccines are the reason that MTHFR C677T variant carriers should not be vaccinated.
There was a small study done showing that people with the MTHFR C677T variant might be more sensitive to mercury. The study looked at the genes of 25 participants that had been diagnosed as sensitive to mercury compared with a control group of 25. The MTHFR 1298C/C genotype was more common in the mercury-sensitive group.
But… Mercury has been removed from children’s vaccinations since 2001 in the U.S. Seasonal flu vaccines for those over 6 years old can still contain mercury, so check the ingredients on that particular vaccine if you are concerned about mercury.
I found no other links between MTHFR variants and other common excipients in vaccines.[ref]
Common vaccine excipients include (according to the CDC):
- egg protein
- formaldehyde (which is also produced in the body)
- sugars
- gelatin
- aluminum salts
- small amounts of antibiotics
A study on vaccines and MTHFR that (hopefully!) doesn’t apply to children found that a cocaine vaccine actually worked better for people with the MTHFR 677 T/T genotype (decreased cocaine use and depression scores).[ref]
Cover-up or a conspiracy?
Perhpaps you are wondering if the link between MTHFR and vaccine injuries is just being covered up — or perhaps deliberately not studied.
But… this doesn’t seem to be the case.
Numerous studies have investigated the interaction between genetics and vaccination reactions.
Adversomics: adverse vaccine reactions research
There is a field of research called ‘adversomics’ which looks into how genetics, epigenetics, and bioinformatics information can be used in analyzing the adverse events from vaccines. [ref]
Vaccine efficacy studies cover how different genetic variants increase or decrease the effectiveness of vaccines as well as how genes interact with adverse events.
Take, for example, a study that found several HLA (human leukocyte antigen) gene variants and other immune system gene variants that do play a role in how vaccines work. The study examined the response to measles vaccinations and found that HLA type reliably predicted whether the recipient would have a strong or weak immune response to the vaccine.[ref] Another study found that CD46 genetic variants also influenced the response to the measles vaccine.[ref]
Related article: 9 Genes that Influence Vaccine Response.
Instead of a conspiracy against the MTHFR variant, researchers focus on genes that actually do impact vaccine response.
Vaccine exemptions for MTHFR:
You may be wondering if you should talk with your doctor about a vaccine exemption for a child with an MTHFR variant. That is, of course, between you and your doctor.
There is no research-backed evidence, though, that I’ve found that indicates that the common MTHFR variants are a reason not to vaccinate.
MTHFR variants are common:
My final point is that the MTHFR C677T and A1298C variants are very common. More than half the population carries one of the variants.
So a common-sense argument is that if these variants were impacting adverse events from vaccines, that would clearly be seen in the data.
Summing up the evidence:
- No scientific evidence pointing to the common MTHFR variants playing a role in vaccination adverse events.
- Carriers of the MTHFR C677T T/T genotype are possibly more likely to react mildly to the type of smallpox vaccine that was used over 10 years ago.
- Not a coverup. Other genetic variants have been found to increase the risk of either adverse events or vaccine effectiveness — and it makes more sense to study those genes in conjunction with vaccination reactions.
New article: Can you get the COVID vaccine if you have MTHFR?
Related Genes and Topics:
COMT Gene
Wondering why your neurotransmitters are out of balance? It could be due to your COMT genetic variants. The COMT gene codes for the enzyme catechol-O-methyltransferase, which breaks down (metabolizes) the neurotransmitters dopamine, epinephrine, and norepinephrine.
Cortisol and HPA Axis Dysfunction
Cortisol is a hormone produced by the adrenal glands in times of stress, and it also plays many roles in your normal bodily functions. Your genes play a big role in how likely you are to have problems with cortisol and HPA axis dysfunction.
Migraines: Genetics and Solutions
Migraines plague more than a billion people worldwide. That is a lot of people who know the pain, mental fogginess, sensitivity to light, and overwhelming desire to crawl into a dark hole and hide from the world. Knowing how your genes influence your risk of migraines can help you tailor solutions that may work better for you.
Initially published July 2017, updated Jan 2021.
References:
Austin, David William, et al. “Genetic Variation Associated with Hypersensitivity to Mercury.” Toxicology International, vol. 21, no. 3, Dec. 2014, pp. 236–41. PubMed, doi:10.4103/0971-6580.155327.
Clifford, Holly D., et al. “CD46 Measles Virus Receptor Polymorphisms Influence Receptor Protein Expression and Primary Measles Vaccine Responses in Naive Australian Children.” Clinical and Vaccine Immunology: CVI, vol. 19, no. 5, May 2012, pp. 704–10. PubMed, doi:10.1128/CVI.05652-11.
Felger, J. C., and F. E. Lotrich. “Inflammatory Cytokines in Depression: Neurobiological Mechanisms and Therapeutic Implications.” Neuroscience, vol. 246, Aug. 2013, pp. 199–229. ScienceDirect, doi:10.1016/j.neuroscience.2013.04.060.
Haralambieva, Iana H., et al. “The Genetic Basis for Interindividual Immune Response Variation to Measles Vaccine: New Understanding and New Vaccine Approaches.” Expert Review of Vaccines, vol. 12, no. 1, Jan. 2013, pp. 57–70. PubMed Central, doi:10.1586/erv.12.134.
Reif, David M., et al. “Genetic Basis for Adverse Events after Smallpox Vaccination.” The Journal of Infectious Diseases, vol. 198, no. 1, July 2008, pp. 16–22. academic.oup.com, doi:10.1086/588670.
—. “Genetic Basis for Adverse Events Following Smallpox Vaccination.” The Journal of Infectious Diseases, vol. 198, no. 1, July 2008, pp. 16–22. PubMed Central, doi:10.1086/588670.
Research, Center for Biologics Evaluation and. “Thimerosal and Vaccines.” FDA, Apr. 2019. www.fda.gov, http://www.fda.gov/vaccines-blood-biologics/safety-availability-biologics/thimerosal-and-vaccines.
Vaccines: Vac-Gen/Additives in Vaccines Fact Sheet. 14 Jan. 2020, https://www.cdc.gov/vaccines/vac-gen/additives.htm.
Zhang, Sarah. “Why Anti-Vax Doctors Are Ordering 23andMe Tests.” The Atlantic, 23 May 2019, https://www.theatlantic.com/science/archive/2019/05/vaccines-dna-23andme/589915/.