Roosters crowing at the first crack of daylight… Morning glories unfurling their blooms as the sun rises in the sky… Fireflies flickering as dusk falls…
It is easy to see that plants respond to sunlight, using photons from the sun to produce energy and store sugar during daylight.
It is easy to also apply the thought of daily rhythms to animals, with nocturnal mice scurrying around at night and diurnal birds chirping in the morning.
Circadian rhythms are hardwired into humans, also.
In fact, all animals and plants are governed by circadian rhythms, from blue-green algae preparing for sunrise to the much more complex organisms with nocturnal (night-active) and diurnal (daytime-active) patterns.[ref]
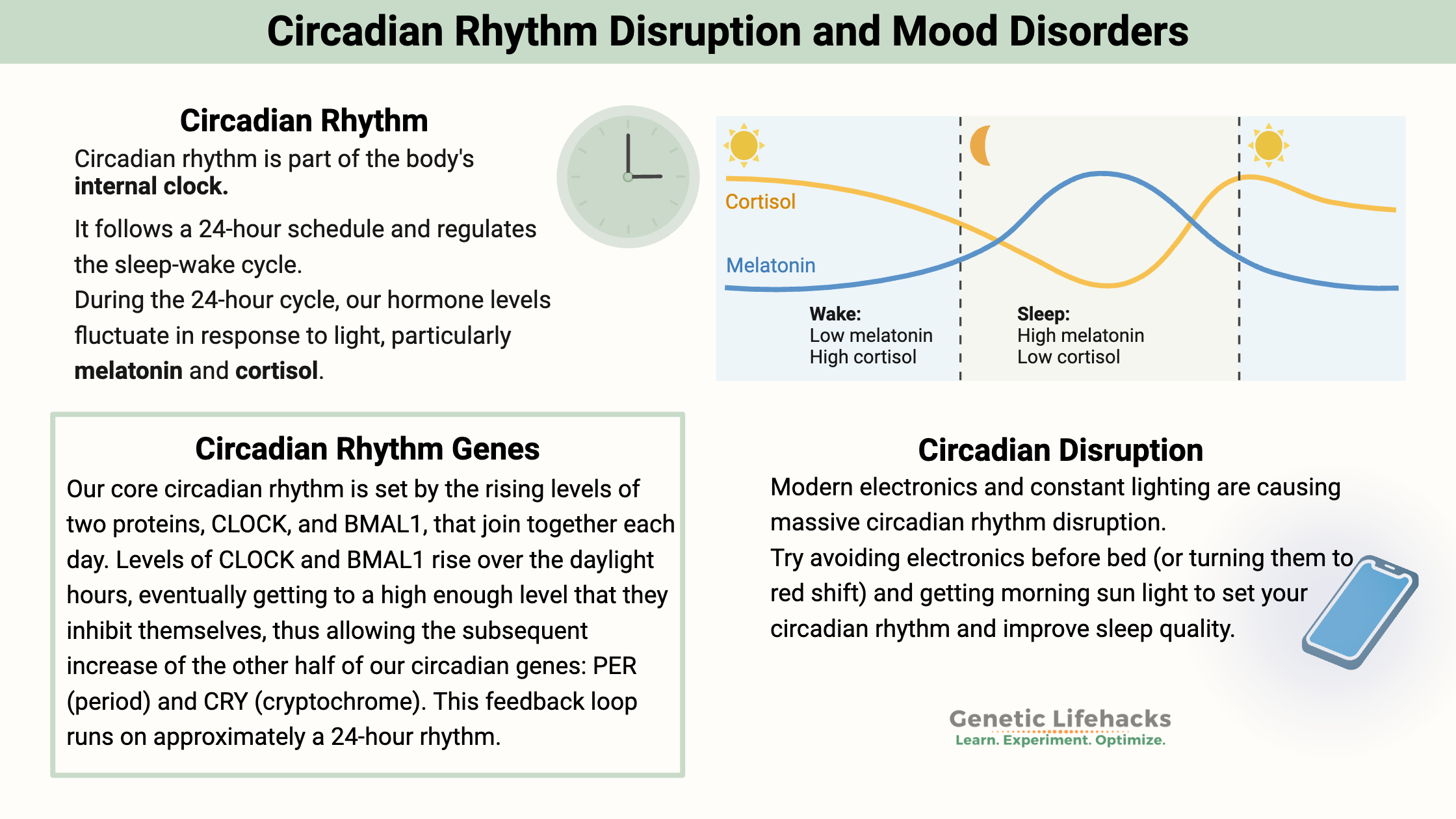
Circadian Rhythm:
Abundant research now shows that our circadian rhythm is fundamentally important to our health.
Our determination to conquer the night, to be a hustling, bustling 24-hour society, is at the root of diseases, including mood disorders, cancers, heart disease, dementia, and diabetes.
Circadian rhythm science goes much deeper than just the standard advice that you should sleep well. Everyone knows that they should sleep well – and most ignore it. Sleep is involved in circadian rhythm, but it is so much more!
How research proves circadian rhythm disruption drives mood disorders:
The flow of science usually starts with observing a phenomenon. It is talked about, poked, and prodded, and theories fly. But a true understanding of a phenomenon or a disease comes with understanding the mechanisms that cause it, essentially reverse-engineering it.
One way of reverse-engineering chronic diseases is to look at the genes that cause an increased risk for a disease. Modeling the disease state can then happen in an animal model using genetic manipulation or knocking out a gene to see the effect.
My path into investigating the impact of circadian rhythms started with diving into genetics and a fascination with the genes that control our core circadian clocks. Humans (like all animals) have a few core genes that regulate our internal rhythms, such as the rise and fall of our hormones, enzyme level fluctuation, cellular repair, body temperature, and the sleep/wake cycle.
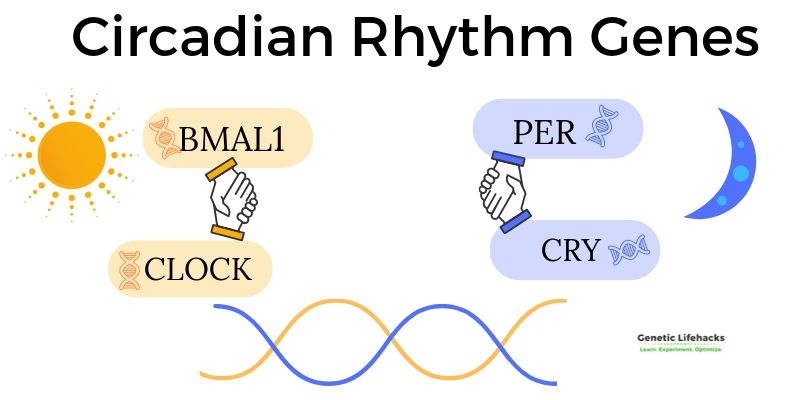
Our core circadian rhythm is set by the rising levels of two proteins, CLOCK, and BMAL1, that join together each day. Levels of CLOCK and BMAL1 rise over the daylight hours, eventually getting to a high enough level that they inhibit themselves, thus allowing the subsequent increase of the other half of our circadian genes: PER (period) and CRY (cryptochrome). This feedback loop runs on approximately a 24-hour rhythm.
Notice the word approximately. Circadian comes from the Latin words circa (about) and dia (day). About a day. The daily fluctuations of our circadian rhythms usually take a little over 24 hours for humans kept in total darkness, and other animals may have slightly shorter than 24-hour periods. The CLOCK and BMAL1 timing need to be regularly set and adjusted.
So what sets the beginning of our daily rhythm? Morning sunlight.
The shorter wavelengths of sunlight in the 450-480nm wavelengths, which we perceive as blue light, are exciting a non-image-forming photoreceptor (melanopsin) in the retina of the eye that signals the beginning of the day. Like a lock and key, the specific wavelength of blue light causes the excitation of the molecule, triggering the signal for our circadian clock. (If you think back to plant biology, this same mechanism is at work in photosynthesis with a specific wavelength of light exciting the chlorophyll pigment inside the chloroplast.)
Rods and cones make up the image-forming photoreceptors in the eye. Researchers discovered about twenty years ago that there is a third type of photoreceptor in the eye known as intrinsically photosensitive retinal ganglion cells (ipRGCs). The blue light-sensitive pigment in these cells is known as melanopsin.[ref]
Lighting up the night – and messing up circadian rhythm
This past century has created huge changes in our circadian rhythm.
- Since cavemen first discovered fire, we have been able to push back the darkness a little bit with a warm glow. Firelight is mainly light in the yellow and red end of the visible light spectrum without any of the shorter, blue wavelengths.
- About 120 years ago, we conquered the night with electric lights, but these incandescent bulbs also cast a warm, yellowish light with only a little in the blue wavelength spectrum.
- Black and white TVs came into living rooms in the ’50s, and by the 1980s, everyone had color TVs pouring blue flickering light out into the night as we sat glued to the Duke of Hazard and The A-Team.
Fast forward to our modern era of ubiquitous electronic devices such as cell phones, tablets, and laptops, all glowing with light in the shorter, blue wavelengths. Add in the effects of LED and compact fluorescent light bulbs, which both have sharp peaks of blue wavelengths in their spectrum.
We are now bombarding the receptors in our retinas at night with light in the exact wavelength (480nm) that signals to our brain that it is daytime.
This constant lighting is causing massive circadian rhythm disruption.
What is the core circadian clock?
All of this core circadian oscillation takes place in a region of the brain called the suprachiasmatic nucleus (SCN). Located in the hypothalamus, the SCN is connected to the retina and receives the signal from the ipRGCs. One interesting fact about the SCN is that when it is isolated from the rest of the brain, the cells still maintain electrical and molecular rhythms – the clock keeps on ticking.[ref]
It helps to visualize the rise and fall of the circadian genes like a sine wave, with the amplitude (height) of the wave being important, as well as the phase (length of time) affecting us.
Research linking circadian rhythm to mood disorders:
Statistics show that 18.3% of US adults suffer from a mental illness, including mood disorders such as depression, anxiety, and bipolar disorder.[ref]
Seasonal Affective Disorder:
Let’s start with an easy and obvious example: Seasonal Affective Disorder (SAD) is a well-known disorder that involves the onset of depressive symptoms with the changing amount of daylight in the fall or winter. SAD affects between 2 – 9% of the population, depending on the latitude. It is now thought that the decreased intensity or brightness of the light is what triggers SAD rather than a shorter period of daylight. One effective therapy for seasonal affective disorder is bright light therapy.[ref] More to read: Genetics of Seasonal Affective Disorder
A study of diurnal (active during daylight) rats found that decreasing the intensity of light could effectively cause anxiety-like behavior. In other words, dim light was causal for mood disturbance. The researchers also found that the decreased light intensity caused a disruption to the HPA axis with increased corticosterone production.[ref] Corticosterone in rodents is equivalent to cortisol production in humans.
Bipolar disorder:
The link between circadian disruption and bipolar disorder has been known since before the 1970s. Bipolar patients with a shortened circadian period are the ones who respond to lithium carbonate, which has recently been shown to inhibit GSK3beta, directly impacting the core clock genes.[ref] Lithium also causes an increase in the amplitude of the production core circadian protein PER2.[ref]
The worldwide lifetime risk of bipolar disorder is a little over 2%, with onset most likely occurring between the ages of 17-27. One mutation in the gene, CLOCK, causes people to be more likely to stay up a little later in the evenings (evening chronotype); it is also linked to a doubling of the risk of bipolar disease.[ref]
Depression:
Major depressive disorder (MDD) has also been linked to circadian disruption. Our neurotransmitter levels of serotonin, norepinephrine, and dopamine all fluctuate with a circadian rhythm over the day. Moreover, MAOA (monoamine oxidase A), which terminates dopamine signaling, is a transcriptional target of the core circadian genes BMAL1 and PER2.[ref]
Related article: MAO-A and MAO-B: Neurotransmitter levels, genetics, and studies
It is interesting to look at how antidepressants work. Studies show that SSRIs shorten or advance the circadian period, and fluoxetine also causes phase advances.[ref] It is thought that SSRIs are increasing serotonin in the SCN (suprachiasmatic nucleus), and part of the reason that it takes a little time for them to be effective is that they are changing the body’s circadian rhythm, which takes a little while to adjust.[ref]
 This brings us back to the chicken or the egg argument. Are mood disorders causing the changes in circadian rhythms, or are altered circadian rhythms causing mood disorders?[ref] There seem to be arguments on both sides, and it could be that both sides are correct in that the interrelated feedback loops could keep driving the dysfunction.[ref]
This brings us back to the chicken or the egg argument. Are mood disorders causing the changes in circadian rhythms, or are altered circadian rhythms causing mood disorders?[ref] There seem to be arguments on both sides, and it could be that both sides are correct in that the interrelated feedback loops could keep driving the dysfunction.[ref]
One strong argument for circadian dysfunction causing mood disorders is that genetic variants in the core circadian genes are linked to an increased risk of major depressive disorder, bipolar disorder, and anxiety. Another strong link is that altering the CLOCK gene in mice can produce a mouse model of depression. One specific strain, called CLOCK delta19 mice, causes a longer circadian period with mania and anxiety during daylight and then a normal mood state when in darkness.[ref] Decreasing the BMAL1 gene in the suprachiasmatic nucleus of mice induced helplessness, behavioral despair, anxiety, and weight gain.[ref]
But not all circadian gene mutations cause mood disorders. Per1 and Per2 mouse mutant strains have altered circadian rhythms without mood alterations. This has led some to hypothesize that light, rather than circadian rhythm, plays a causal role in mood disorders.[ref] While a genetic variant of the CLOCK gene may double the risk of bipolar disorder, obviously, not everyone with the variant will become bipolar.[ref]
Looking at animal models of depression adds more fuel to both sides of the argument. Chronic mild stress causes a dampening in the amplitude of circadian rhythms in mice. It also causes damping of amplitudes of daily temperature variations and corticosterone production.[ref]
What do human studies show?
Shift workers who alter their schedules for work are at an increased risk for depression.[ref] While the numbers vary depending on the study, a 2017 meta-analysis came up with a conservative estimate of a 43% increase in the risk of depression for those who work the night shift.[ref]
A number of human core clock genes are associated with the risk of MDD and seasonal affective disorder. Again, finding that circadian gene variants can cause mood disorders is a strong indicator that circadian disruption drives mood disorders. Recently, it was shown that a PER3 mutation that causes Familial Advanced Sleep Phase Disorder (people who have this naturally want to go to sleep very early in the evening and get up extremely early in the morning) also is causal for seasonal affective disorder. The same study created a mouse model that decreased PER3 expression, which showed that not only were the mice depressed, but the severity of depression was worse with a shorter photoperiod.[ref]
A study of patients with depression looked at the gene expression at the time of death (you can’t do a lot of in vivo studies on gene expression in the brain with people who are living). The study found that compared to non-depressed, people with depression controls who had died at the same time of day showed a phase delay in gene expression, strongly linking circadian rhythm changes to depression.[ref]
Sleep disturbance goes along with altered circadian rhythms, and sleep disturbances are a hallmark of both bipolar disorder and depression. It is theorized that dampened and shifted circadian rhythms can explain sleep disturbances in mood disorders. Indeed, dampened temperature fluctuations (our body temperature is supposed to drop at night) and dampened hormonal rhythms are a big part of depression. In bipolar patients, it has been shown that circadian gene expression is phase advanced in manic states and delayed during periods of depression.[ref]
A recent study of blue-blocking glasses for bipolar patients had very positive results. The study used two groups of patients, one group wearing blue-blocking glasses from 6 pm to 8 am for seven days, while the other group wore clear lenses. After seven days, the group wearing blue-blocking glasses had a drop in the Young Mania Rating Scale of 14.1 compared to the placebo group, which had a drop of 1.7.[ref] Simple, inexpensive, and effective – blocking blue light in the evenings had a significant impact after only a week.
Let me wrap this up by pointing out some things that may seem obvious now:
- We are a society that is chronically somewhat stressed.
- Most of us spend the majority of our day inside with low amounts of light (compared to sunlight).
- We are constantly telling our bodies that it is morning instead of night through our use of electronic devices, with blue light hitting our eyes at night.
- All of this has a deleterious effect on our circadian rhythm.
Lifehacks:
Block the Blue Light at Night:
Blue-blocking glasses (amber or orange-colored lenses) in the evening for a couple of hours before bedtime. This means wearing them constantly since less than a minute of blue light can delay melatonin onset for quite a while. One study found a 50% increase in melatonin production after just two weeks of wearing blue-blocking glasses.[ref] Be sure to look for ones that block 100% of the blue light wavelengths.
Alternatively, you could stop watching TV in the evenings, avoid reading from a lighted eReader and refrain from looking at your cell phones, tablets, and laptops. Couple the avoidance of all electronics with low lighting in your house from bulbs that have a red hue, and you are on the right track to resetting your circadian clock.
Bright Light During the Day:
Sunlight during the daytime is really important. There is just no way to get enough brightness from normal light bulbs during the day. Try eating your breakfast and lunch outside, or park farther from work and walk in the sunshine for a bit before your day begins. Just make it a priority to get some sunlight. A study shows that even sitting next to a window in your office can help.[ref] Another study found that increasing morning light decreased depression and increased sleep quality.[ref]
Light therapy devices are becoming more and more prevalent, and the studies on them are showing efficacy for more than just seasonal affective disorder. One recent clinical trial found light therapy effective for postpartum depression, and another in dementia patients also found bright light therapy effective.[ref][ref] There are literally a couple of thousand studies available on light therapy for depression, so I would encourage you to research the topic. Note that for most studies on depressed patients, the participants continued their current depression medication during the trial. If you are currently on medication, please don’t just throw out your bottle of pills and turn on a bright light—talk with your doctor and come up with a plan.
Darkness at Night:
Dark Therapy has been tried for some bipolar patients, with forced darkness for 10 hours per night leading to stabilization in mood.[ref] Along those same lines, all of us can benefit from blocking out all light sources in our bedrooms while we sleep. Get some blackout curtains (inexpensive online), and cover up all the little LED lights on chargers, etc.
Final thoughts:
Read and learn more, pay attention to your circadian rhythm, and realize that the inconvenience of staying on a normal sleep/wake routine more than pays off in benefits for your long-term mental and physical health.
Related Articles and Topics:
References: