Key takeaways:
~ Cold sores are caused by the herpes simplex virus (HSV).
~ Less than half of people with HSV will get cold sores from the virus.
~ Genetics plays a role in who will get cold sores, and environmental factors can trigger the occurrence.
What causes cold sores?
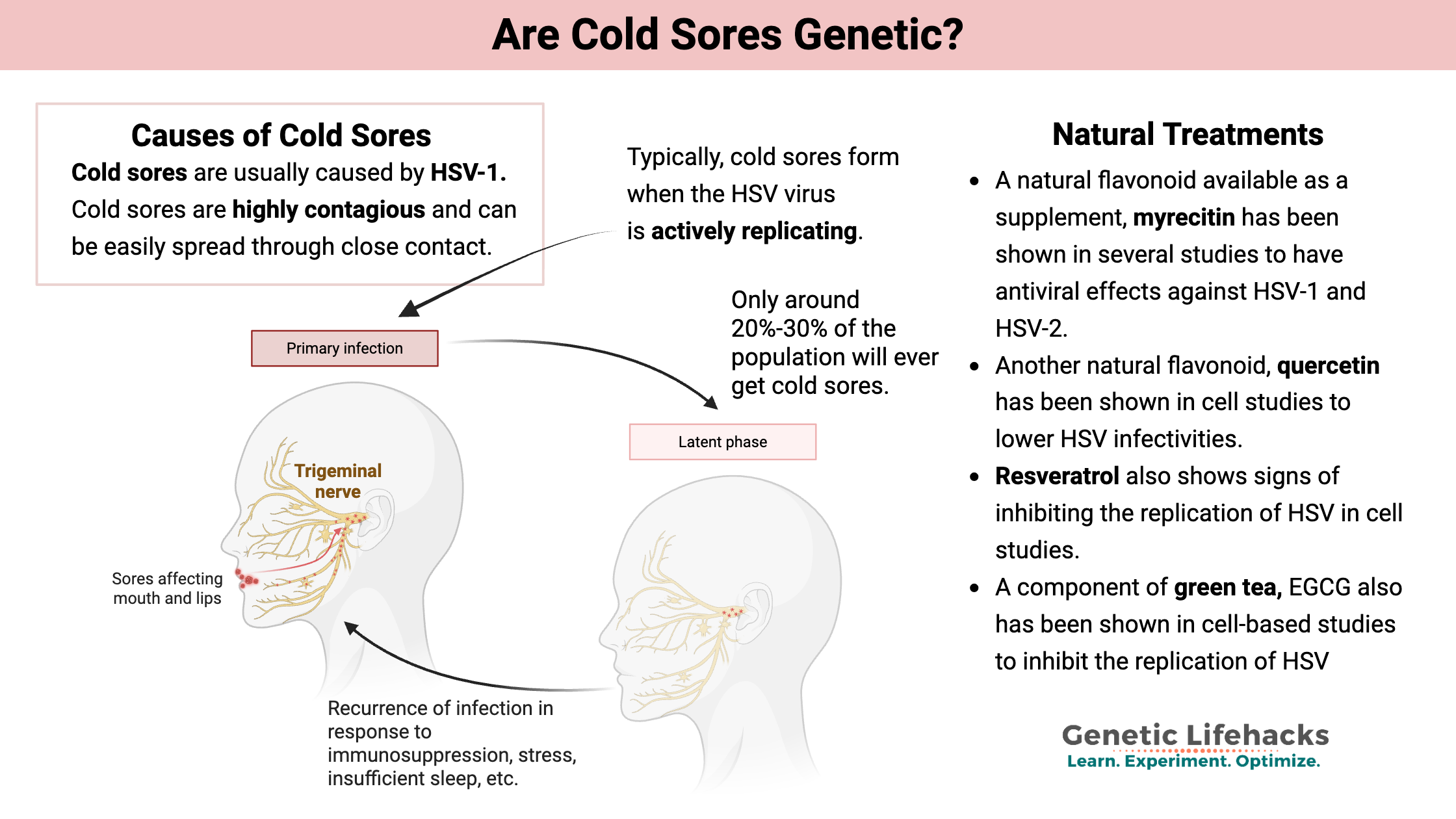
There are two types of herpes simplex virus: HSV-1 and HSV-2. Cold sores are usually caused by HSV-1, while HSV-2 usually causes genital herpes. But, either type of HSV can cause either condition.

Once the herpes simplex virus enters your body, it stays for life. It hides in nerve cells and can become active again later, causing another outbreak of cold sores.
Cold sores are highly contagious and can be easily spread through close contact, such as kissing or sharing utensils. If you have a cold sore, it’s important to avoid close contact with others, especially newborns, and to wash your hands frequently to prevent spreading the virus.
Using DNA from people who lived in the Bronze Age, researchers now think that HSV-1 has been making the rounds in humans for around 5,000 years.[ref]
Science of cold sores
Cold sores are also called herpes simplex labialis or fever blisters.
About 60%-80% of the population is seropositive for HSV1, but only around 20%-30% of the population will ever get cold sores. Some people get a cold sore rarely (once or twice a decade), while others may have monthly outbreaks.[ref][ref]
The sores that form on the outside or inside of the lip are uncomfortable — and embarrassing for some people. Who wants an open sore or big scab on their lip…
Typically, cold sores form when the HSV virus is actively replicating. Often people notice tingling or burning in the affected area before the development of the sore. Rupturing of the blister that forms will lead to a scab.[ref]
Why does this happen? The virus infects nerves around the mouth and remains latent in the nucleus of neurons, undetected by your immune system. When reactivated, the virus creates new infectious particles that move down the neuron to the skin, causing the sores.
Interestingly, the latent virus is thought to enhance the survival of the infected cells.
What causes the reactivation of the virus?
Triggers of HSV reactivation include:[ref]
- stress, which can alter immune response
- ultraviolet (UV) radiation (sunburn)
- temperature fluctuations (cold, wind, heat)
- surgical trauma or dental procedures
- immunotherapy that suppresses the immune response
- hormonal changes
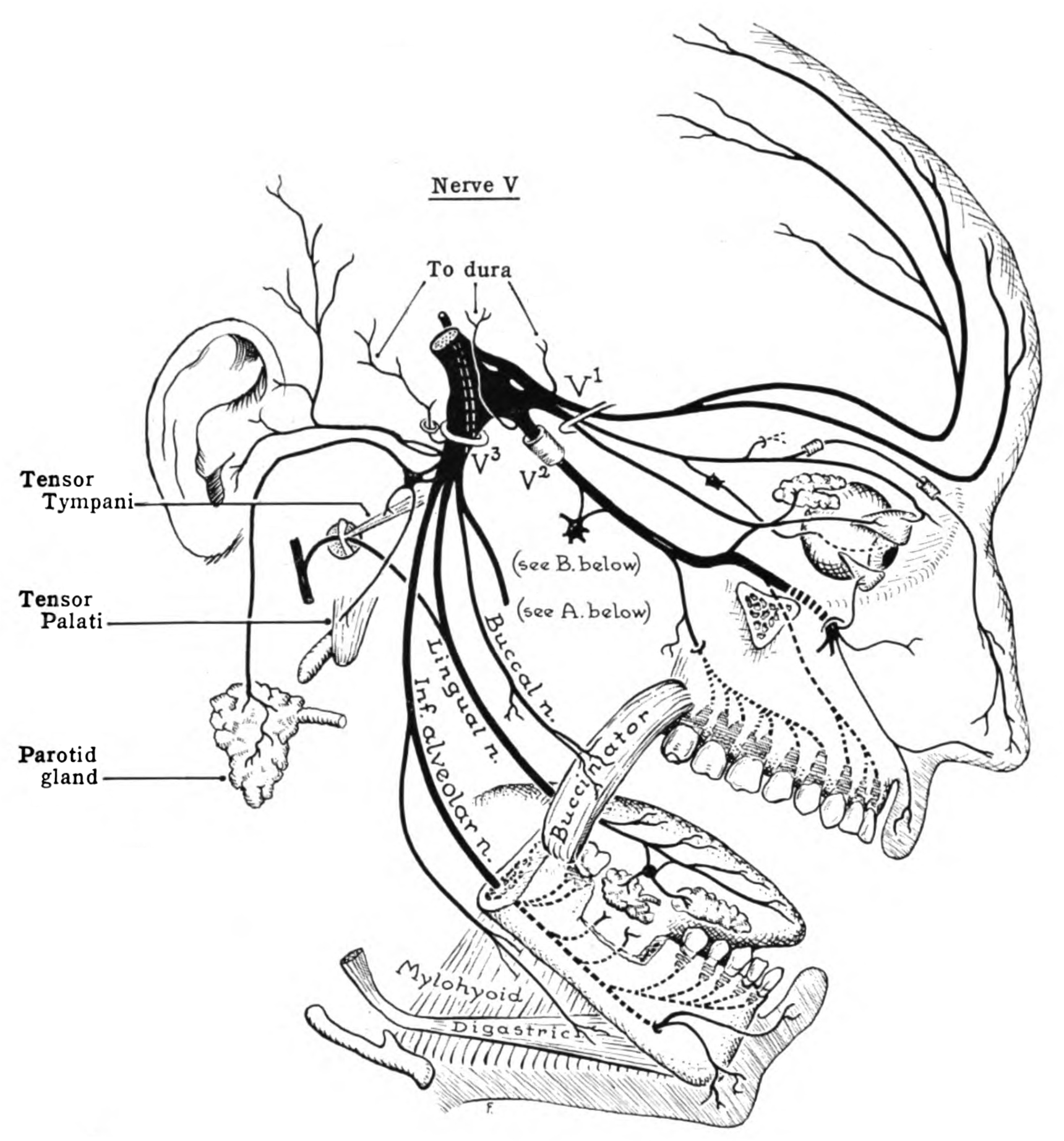
Researchers find that HSV-1 reactivates in the trigeminal nerve when the immune system is suppressed, such as during times of stress or when fighting off another infection.
Why doesn’t everyone with HSV get cold sores?
This is a question that researchers have been trying to answer for decades.
Genetics is at least part of the answer as to why everyone doesn’t get cold sores. The strain of the herpes simplex virus may play a role as well. Additionally, an external stressor such as wind, sunburn, or oral surgery may need to be involved for some to activate the virus.[ref][ref]
Keep in mind that not everyone gets the herpes simplex virus. Transmission of the virus is usually through skin contact and is more likely if there is slight damage to the surface of the skin.[ref] Additionally, genetic variants in the immune response genes may protect some individuals from ever getting the virus.[ref]
Cold Sores Genotype Report:
Access this content:
An active subscription is required to access this content.
Lifehacks: Cold Sore Solutions
Talk with your doctor about the pros and cons of prescription-based antiviral medications for cold sores.
The rest of this article is for Genetic Lifehacks members only. Consider joining today to see the rest of this article.
Natural treatments for cold sores:
Access this content:
An active subscription is required to access this content.
Related Articles and Topics:
Breast Implant Illness: The Interplay of Genetics and Symptoms
TNF-alpha: Inflammation, Chronic Diseases, and Genetic Susceptibility
References:
Brancher, João Armando, et al. “Single Nucleotide Polymorphism in Interleukin 1 Alpha Gene Might Be Involved in the Oral Herpes Recurrent Episodes in Brazilian Para-Athletes.” Research, Society and Development, vol. 10, no. 16, Dec. 2021, pp. e564101624166–e564101624166. rsdjournal.org, https://doi.org/10.33448/rsd-v10i16.24166.
Danileviciene, Vilija, et al. “The Role of C21orf91 in Herpes Simplex Virus Keratitis.” Medicina (Kaunas, Lithuania), vol. 55, no. 12, Nov. 2019, p. 753. PubMed, https://doi.org/10.3390/medicina55120753.
Gopinath, Divya, et al. “A Comprehensive Overview of Epidemiology, Pathogenesis and the Management of Herpes Labialis.” Viruses, vol. 15, no. 1, Jan. 2023, p. 225. PubMed Central, https://doi.org/10.3390/v15010225.
Jamgochian, Marielle, et al. “Diet in Dermatology: Review of Diet’s Influence on the Conditions of
Rosacea, Hidradenitis Suppurativa, Herpes Labialis, and Vitiligo.” American Journal of Lifestyle Medicine, vol. 17, no. 1, July 2021, pp. 152–60. PubMed Central, https://doi.org/10.1177/15598276211026592.
Kreier, Freda. “Ancient Tooth DNA Reveals How ‘Cold Sore’ Herpes Virus Has Evolved.” Nature, vol. 609, no. 7925, Aug. 2022, pp. 21–22. www.nature.com, https://doi.org/10.1038/d41586-022-02246-1.
Kriesel, John D., Brandt B. Jones, et al. “C21orf91 Genotypes Correlate With Herpes Simplex Labialis (Cold Sore) Frequency: Description of a Cold Sore Susceptibility Gene.” The Journal of Infectious Diseases, vol. 204, no. 11, Dec. 2011, pp. 1654–62. PubMed Central, https://doi.org/10.1093/infdis/jir633.
Kriesel, John D., Amiteshwar Bhatia, et al. “Cold Sore Susceptibility Gene-1 Genotypes Affect the Expression of Herpes Labialis in Unrelated Human Subjects.” Human Genome Variation, vol. 1, no. 1, Nov. 2014, pp. 1–6. www.nature.com, https://doi.org/10.1038/hgv.2014.24.
Lee, Seulki, et al. “The Anti-HSV-1 Effect of Quercetin Is Dependent on the Suppression of TLR-3 in Raw 264.7 Cells.” Archives of Pharmacal Research, vol. 40, no. 5, May 2017, pp. 623–30. PubMed, https://doi.org/10.1007/s12272-017-0898-x.
Mailoo, Venthan J., and Sanketh Rampes. “Lysine for Herpes Simplex Prophylaxis: A Review of the Evidence.” Integrative Medicine (Encinitas, Calif.), vol. 16, no. 3, June 2017, pp. 42–46.
Polansky, Hanan, et al. “Clinical Trial of Herbal Treatment Gene-Eden-VIR/Novirin in Oral Herpes.” Journal of Evidence-Based Integrative Medicine, vol. 23, 2018, p. 2515690X18806269. PubMed, https://doi.org/10.1177/2515690X18806269.
Santamaria, Pasquale, et al. “Associations between Host Genetic Variants and Herpes Simplex Labialis in the TwinsUK Cohort.” Archives of Oral Biology, vol. 145, Jan. 2023, p. 105587. PubMed, https://doi.org/10.1016/j.archoralbio.2022.105587.
Šudomová, Miroslava, et al. “Flavonoids Target Human Herpesviruses That Infect the Nervous System: Mechanisms of Action and Therapeutic Insights.” Viruses, vol. 14, no. 3, Mar. 2022, p. 592. www.mdpi.com, https://doi.org/10.3390/v14030592.
Tian, Chao, et al. “Genome-Wide Association and HLA Region Fine-Mapping Studies Identify Susceptibility Loci for Multiple Common Infections.” Nature Communications, vol. 8, no. 1, Sept. 2017, p. 599. www.nature.com, https://doi.org/10.1038/s41467-017-00257-5.
Wu, Ching-Yi, et al. “Effects of Epigallocatechin-3-Gallate and Acyclovir on Herpes Simplex Virus Type 1 Infection in Oral Epithelial Cells.” Journal of the Formosan Medical Association = Taiwan Yi Zhi, vol. 120, no. 12, Dec. 2021, pp. 2136–43. PubMed, https://doi.org/10.1016/j.jfma.2020.12.018.
Zhu, Shuyong, and Abel Viejo-Borbolla. “Pathogenesis and Virulence of Herpes Simplex Virus.” Virulence, vol. 12, no. 1, pp. 2670–702. PubMed Central, https://doi.org/10.1080/21505594.2021.1982373. Accessed 27 Feb. 2023.