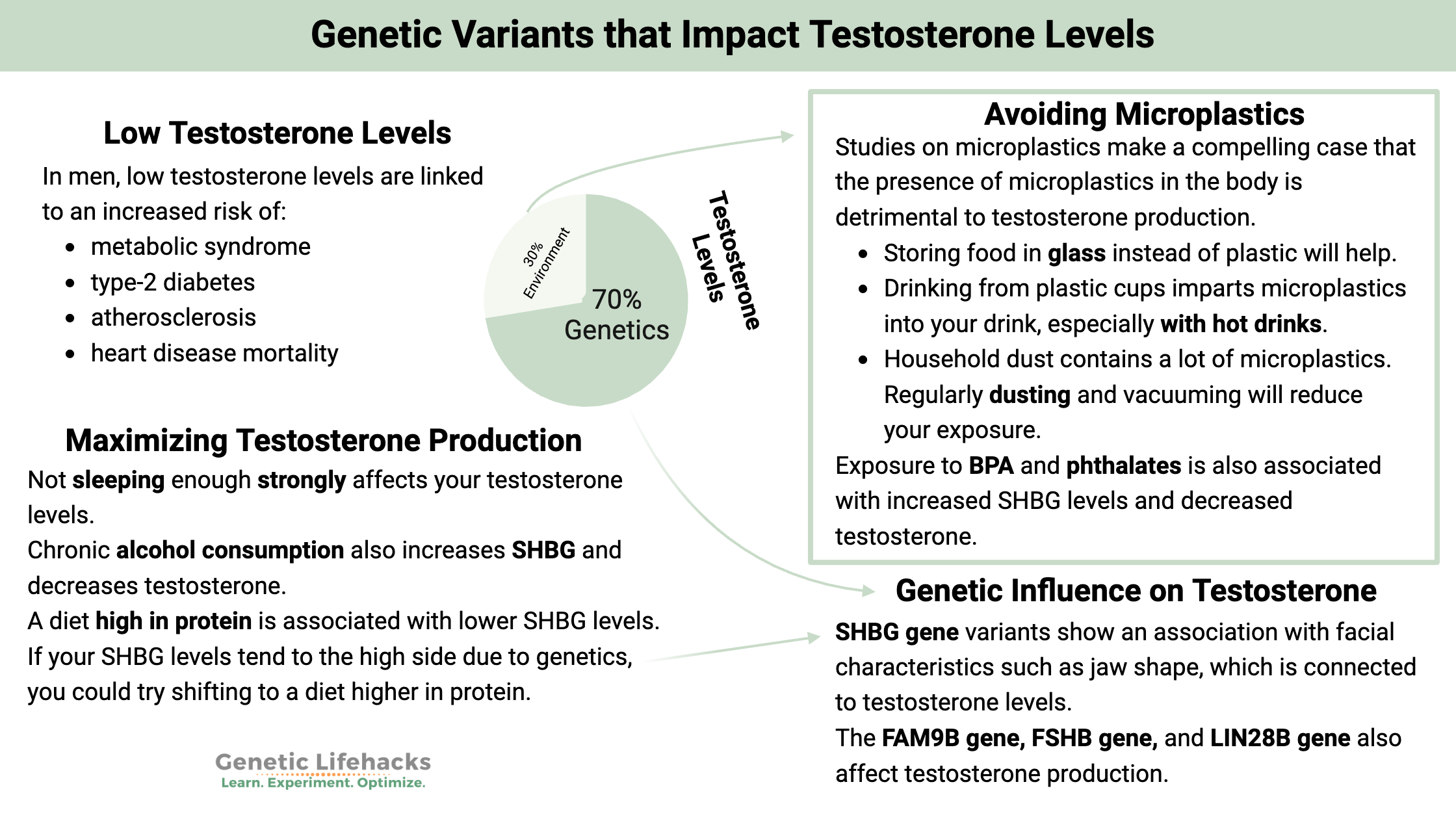
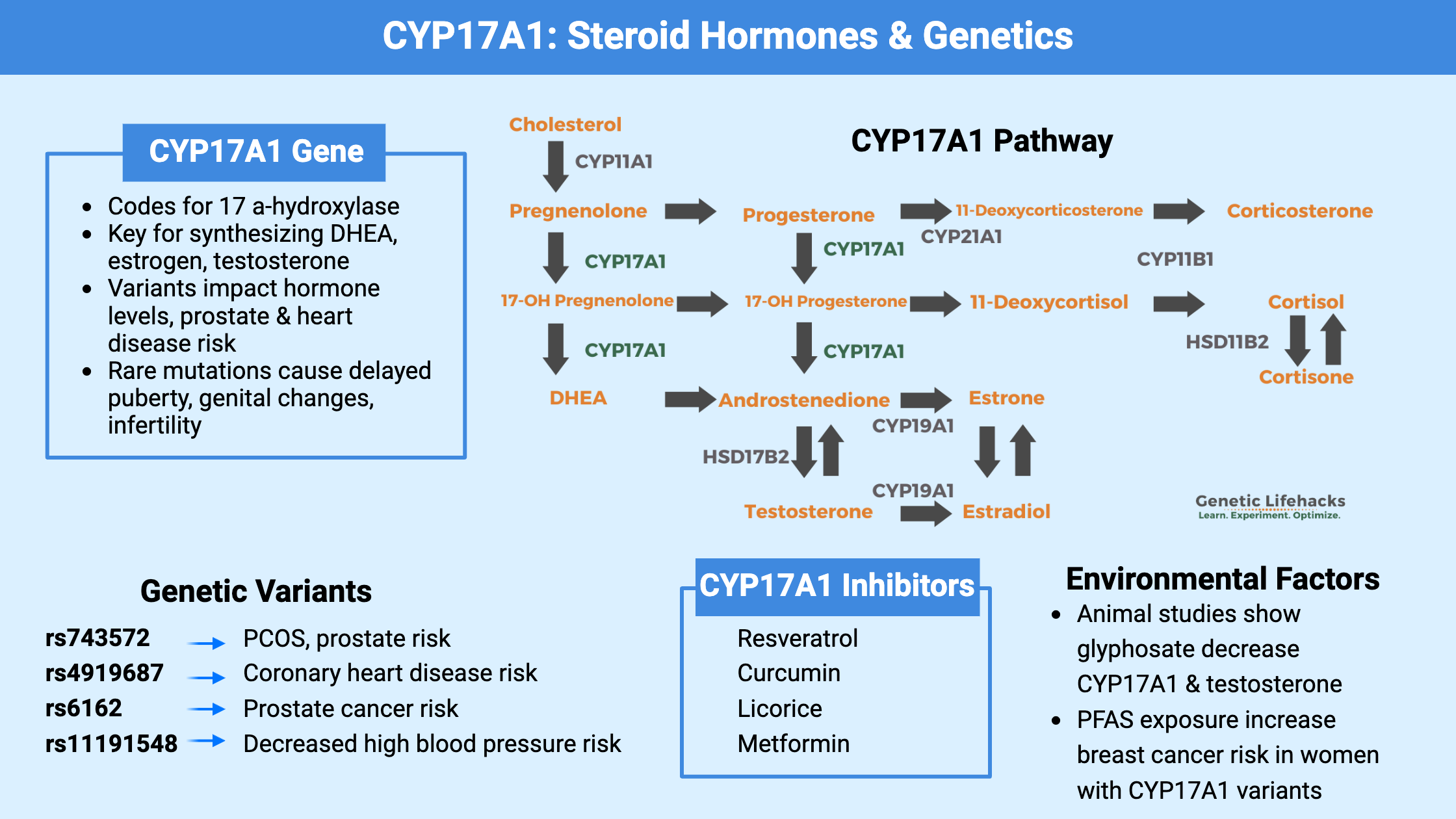
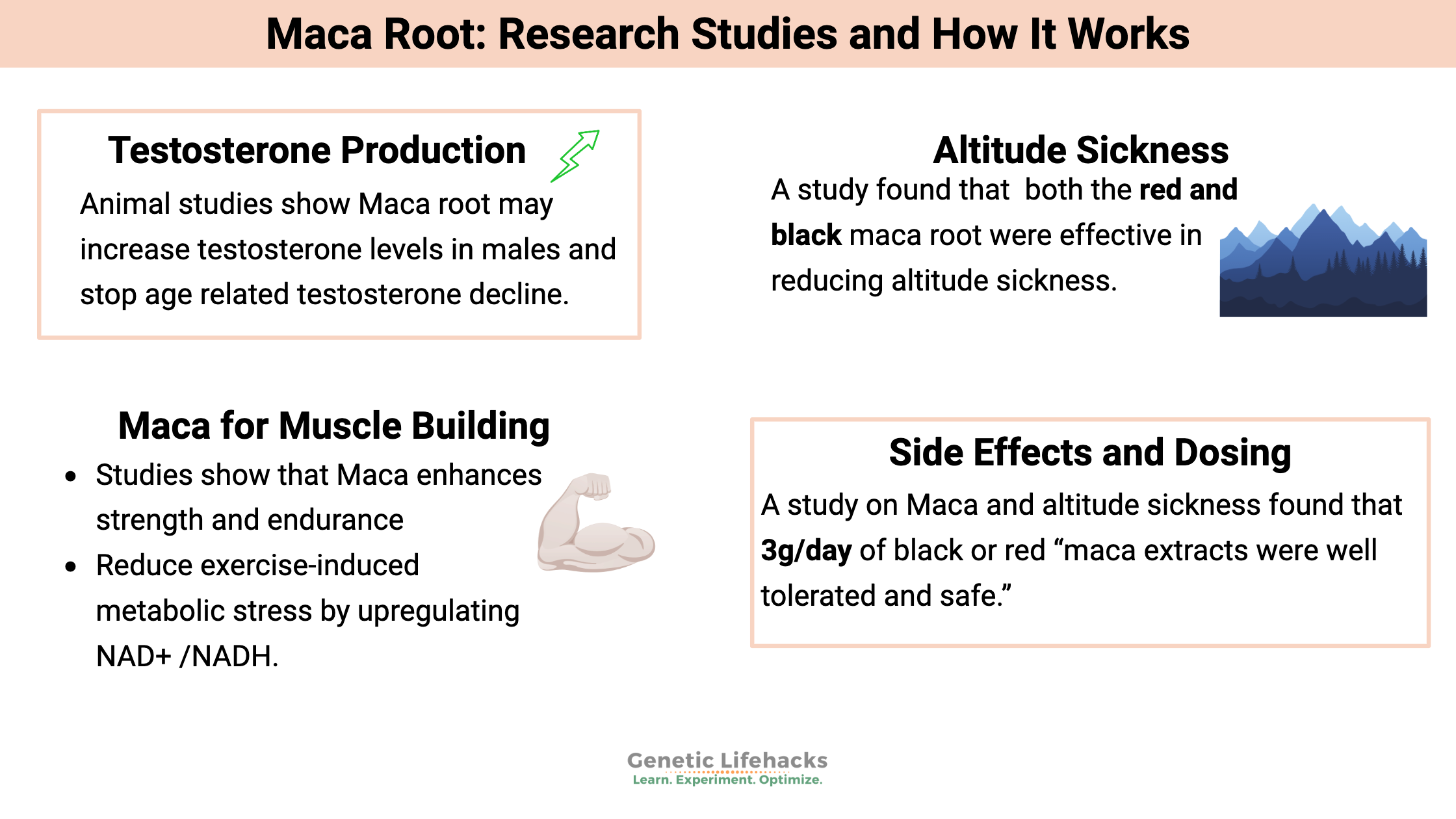
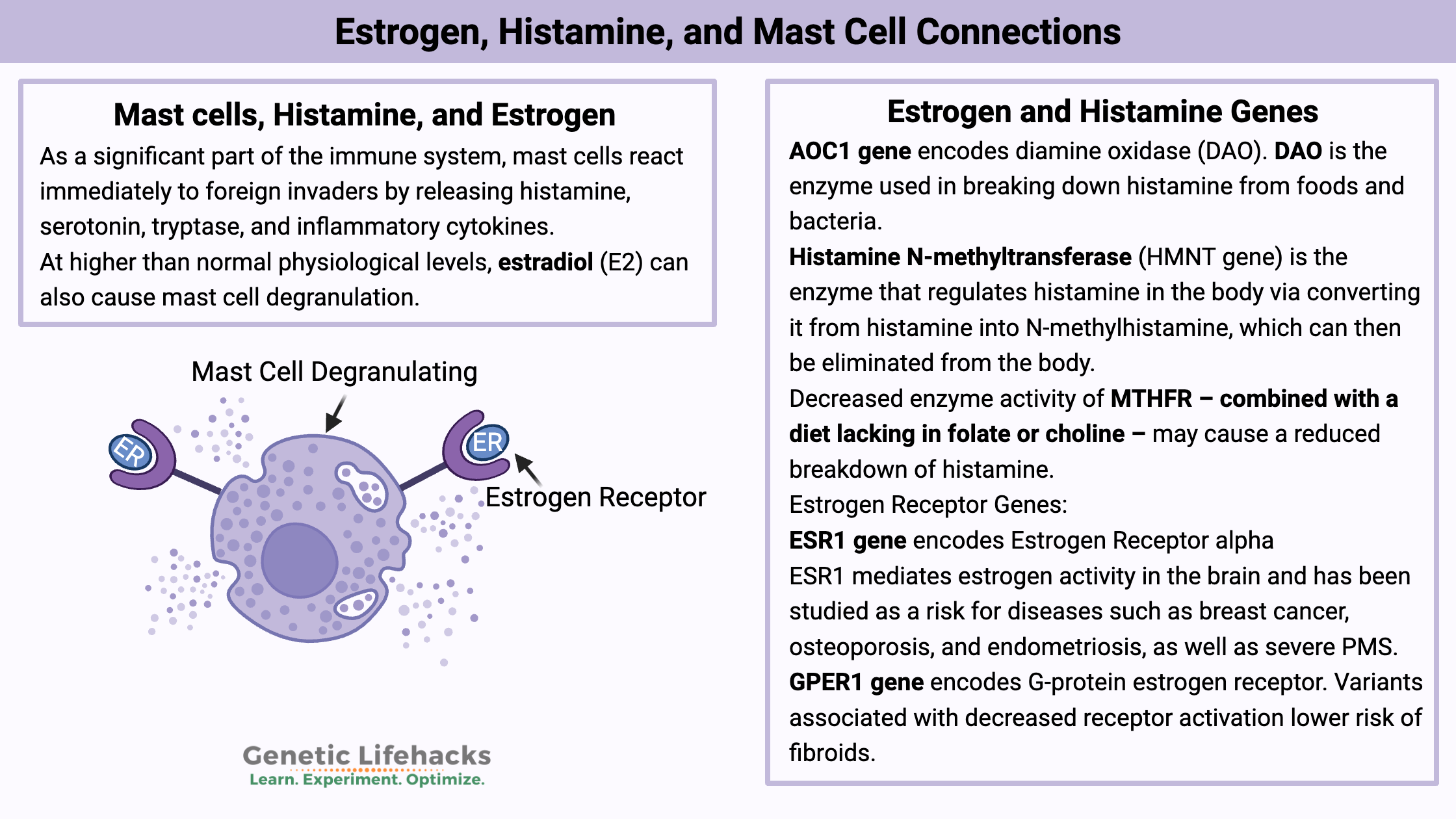
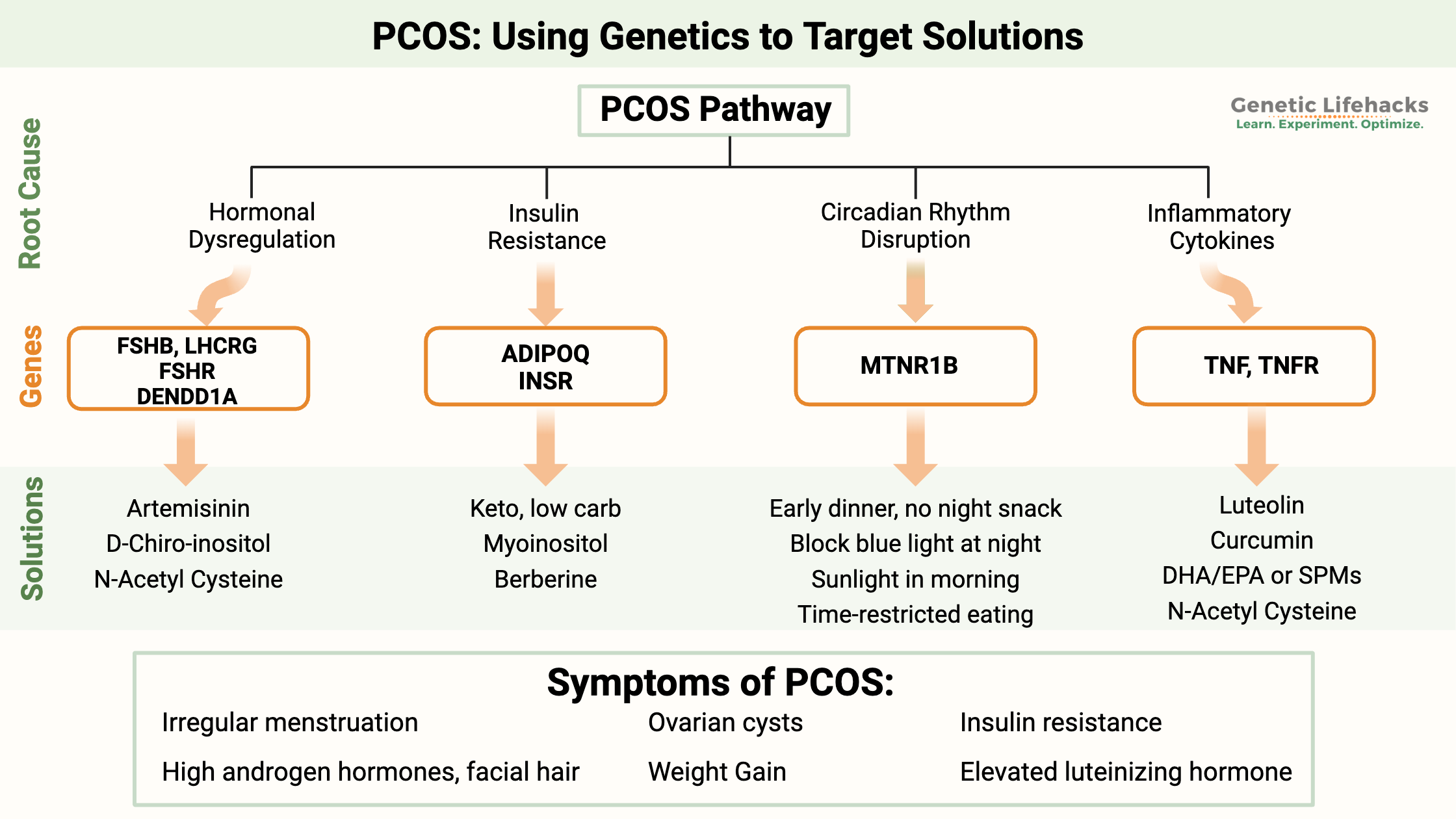
Testosterone: Genetic Variants that Impact Testosterone Levels
While diet and lifestyle play a role in testosterone levels, in males, there is a strong genetic component as well. Check out your genes to see if they are playing a role in your low T levels — and then check out the Lifehacks.